Journal Description
Audiology Research
Audiology Research
is an international, scientific, peer-reviewed, open access journal on audiology and neurotology, published bimonthly online by MDPI (from Volume 10, Issue 2 - 2020). The Italian Society of Vestibology (VIS) is affiliated with Audiology Research and its members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 22.9 days after submission; acceptance to publication is undertaken in 3.7 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.7 (2022);
5-Year Impact Factor:
1.6 (2022)
Latest Articles
Cochlear Implantation in Children Affected by Single-Sided Deafness: A Comprehensive Review
Audiol. Res. 2024, 14(1), 77-85; https://doi.org/10.3390/audiolres14010007 - 12 Jan 2024
Abstract
Children with single-sided deafness (SSD) may experience delays in language and speech development. Reduced speech discrimination and poor sound localization abilities in young SSD patients may result in greater cognitive efforts required to focus and process auditory information, as well as increased listening-related
[...] Read more.
Children with single-sided deafness (SSD) may experience delays in language and speech development. Reduced speech discrimination and poor sound localization abilities in young SSD patients may result in greater cognitive efforts required to focus and process auditory information, as well as increased listening-related fatigue. Consequently, these children can have a higher risk of academic failure and are often in need of extra help at school. Recently, cochlear implants (CIs) have been introduced as a rehabilitative option for these children, but their effectiveness is still a topic of debate. A literature review was performed according to PRISMA guidelines, searching the Medline database from inception to October 2023. The research identified nine papers that met the inclusion criteria. Data extracted from the selected studies included 311 children affected by SSD and cochlear implants. The reported audiological outcomes were further analyzed. Overall, a high level of satisfaction was described by parents of children with SSD and CI, and those who received a CI under the age of 3 presented better results. However, a proportion of patients did not use the device daily. Our review highlights the possible, and still controversial, role of CI for the hearing rehabilitation of children with unilateral deafness, underlining the need for further research in this field. To date, careful and comprehensive counseling with the child and the family is necessary before considering this option.
Full article
(This article belongs to the Collection Cochlear Implants: Challenges and Opportunities in Hearing Rehabilitation)
►
Show Figures
Open AccessArticle
Suspicion and Treatment of Perilymphatic Fistula: A Prospective Clinical Study
Audiol. Res. 2024, 14(1), 62-76; https://doi.org/10.3390/audiolres14010006 - 08 Jan 2024
Abstract
Background: Since the discovery of the perilymphatic fistula (PLF), the diagnosis and treatment remain controversial. If successfully recognized, the PLF is surgically repairable with an obliteration of the fistula site. Successful treatment has a major impact on patient’s quality of life with an
[...] Read more.
Background: Since the discovery of the perilymphatic fistula (PLF), the diagnosis and treatment remain controversial. If successfully recognized, the PLF is surgically repairable with an obliteration of the fistula site. Successful treatment has a major impact on patient’s quality of life with an improvement in their audiological and vestibular symptoms. Objective: To prospectively investigate patients’ clinical and audiological evolution with PLF suspicion after middle ear exploration and obliteration of the round and oval window. Study Design: Prospective comparative study. Setting: Tertiary care center. Methods: Patients were divided into two groups: Group I consisted of patients where no PLF had been identified intraoperatively at the oval and/or at the round window, and Group II consisted of patients where a fistula had been visualized. Patient assessment was a combination of past medical history, the presence of any risk factors, cochlear and vestibular symptoms, a physical examination, temporal bone imaging, audiograms, and a videonystagmogram (VNG). Results: A total of 98 patients were divided into two groups: 62 in Group I and 36 in Group II. A statistically significant difference regarding gender was observed in Group II (83.3% of males vs. 16.7% of females, p = 0.008). A total of 14 cases (4 and 10 in Groups I and II, respectively) were operated for a recurrent PLF. Fat graft material was used in the majority of their previous surgery; however, no difference was found when comparing fat to other materials. In addition, no statistically significant difference was noted between Groups I and II concerning predisposing factors, imaging, VNG, symptom evolution, or a physical exam before the surgery and at 12 months post-operative. However, both groups showed statistically significant hearing and vestibular improvement. On the other hand, the air conduction (AC) and bone conduction (BC) at each frequency were not statistically different between the two groups before surgery but showed statistically significant improvement at 12 months post-operatively, especially for the BC at the frequencies 250 (p = 0.02), 500 (p = 0.0008), and 1000 Hz (p = 0.04). Conclusions: Whenever you suspect a perilymphatic fistula, do not hesitate to explore middle ear and do window obliterations using a tragal perichondrium material. Our data showed that cochlear and vestibular symptoms improved whether a fistula had been identified or not.
Full article
(This article belongs to the Special Issue Inner Ear Conductive Hearing Loss: Current Studies and Controversies)
►▼
Show Figures
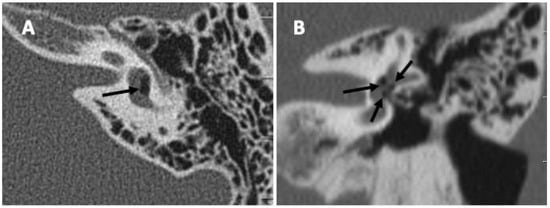
Figure 1
Open AccessReview
Incidence of Otolaryngological Manifestations in Individuals with Autism Spectrum Disorder: A Special Focus on Auditory Disorders
by
, , , , , , , and
Audiol. Res. 2024, 14(1), 35-61; https://doi.org/10.3390/audiolres14010005 - 04 Jan 2024
Abstract
Autism Spectrum Disorder (ASD) is a neurodevelopmental disorder characterized by stereotyped and repetitive behavior patterns. In addition to neurological and behavioral problems, individuals with ASD commonly experience otolaryngological comorbidities. Individuals with ASD often have auditory disorders including hearing loss and auditory processing disorders
[...] Read more.
Autism Spectrum Disorder (ASD) is a neurodevelopmental disorder characterized by stereotyped and repetitive behavior patterns. In addition to neurological and behavioral problems, individuals with ASD commonly experience otolaryngological comorbidities. Individuals with ASD often have auditory disorders including hearing loss and auditory processing disorders such as central auditory processing disorder (CAPD), as well as both chronic and recurrent otitis media. These challenges negatively impact a person’s ability to effectively communicate and may further impact their neurological functioning, particularly when not appropriately treated. Individuals diagnosed with ASD also have difficulty sleeping which contributes to increased irritability and may further aggravate the core behavioral symptoms of autism. The individuals with ASD also have a higher rate of sinusitis which contributes to the worsening of the autism behavior phenotype. The high prevalence of otolaryngological comorbidities in individuals with ASD warrants a better collaboration between their various healthcare providers and otolaryngologists with expertise in auditory, sleep, and sinus disorders in pursuit of improving the quality of life of affected individuals and their families/caregivers.
Full article
(This article belongs to the Special Issue Auditory Disorders: Incidence, Intervention and Treatment)
►▼
Show Figures
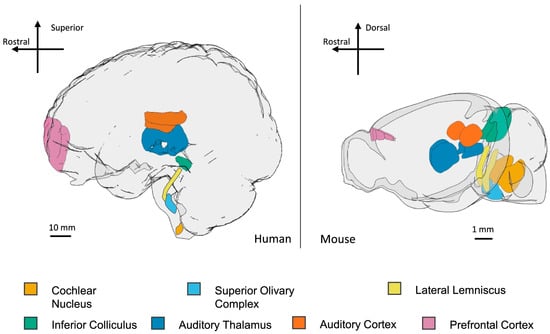
Figure 1
Open AccessArticle
Vestibular Drop Attack: An Analysis of the Therapeutic Response
Audiol. Res. 2024, 14(1), 27-34; https://doi.org/10.3390/audiolres14010004 - 27 Dec 2023
Abstract
The present study evaluates the response to betahistine in patients who presented vestibular drops attacks in the context of Ménière’s disease (MD) and the factors that can predict an unfavorable response to it. A total of 43 patients were analyzed, out of which
[...] Read more.
The present study evaluates the response to betahistine in patients who presented vestibular drops attacks in the context of Ménière’s disease (MD) and the factors that can predict an unfavorable response to it. A total of 43 patients were analyzed, out of which 33 were diagnosed with MD. This is a descriptive, cross-sectional study with retrospective data collection. Data as regards age, accompanying symptoms, etiological diagnosis and response to MD treatment were collected. A statistical analysis was carried out, and we found that the disease evolution time and specific alterations in the vestibulospinal and oculomotor physical examination present an unfavorable response to betahistine. Failures for betahistine were treated with intratympanic gentamicin, with which symptomatic control was achieved in all cases.
Full article
(This article belongs to the Special Issue The beside Evaluation of the Patient with Acute Vertigo: From Ocular to Vestibulo-Spinal Signs)
►▼
Show Figures
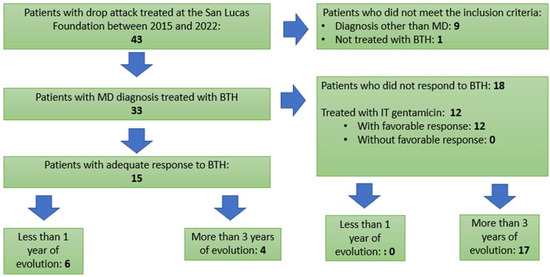
Figure 1
Open AccessComment
Comment on Tabet et al. Vestibular Migraine versus Méniere’s Disease: Diagnostic Utility of Electrocochleography. Audiol. Res. 2023, 13, 12–22
Audiol. Res. 2024, 14(1), 26; https://doi.org/10.3390/audiolres14010003 - 25 Dec 2023
Abstract
I wish to comment on an aspect of the recently published article by Saliba I. et al., titled Vestibular Migraine versus Meniere’s Disease: Diagnostic Utility of Electrocochleograpy [...]
Full article
Open AccessFeature PaperArticle
Waardenburg Syndrome: The Contribution of Next-Generation Sequencing to the Identification of Novel Causative Variants
by
, , , , , , , , and
Audiol. Res. 2024, 14(1), 9-25; https://doi.org/10.3390/audiolres14010002 - 21 Dec 2023
Abstract
Waardenburg syndrome (WS) is characterized by hearing loss and pigmentary abnormalities of the eyes, hair, and skin. The condition is genetically heterogeneous, and is classified into four clinical types differentiated by the presence of dystopia canthorum in type 1 and its absence in
[...] Read more.
Waardenburg syndrome (WS) is characterized by hearing loss and pigmentary abnormalities of the eyes, hair, and skin. The condition is genetically heterogeneous, and is classified into four clinical types differentiated by the presence of dystopia canthorum in type 1 and its absence in type 2. Additionally, limb musculoskeletal abnormalities and Hirschsprung disease differentiate types 3 and 4, respectively. Genes PAX3, MITF, SOX10, KITLG, EDNRB, and EDN3 are already known to be associated with WS. In WS, a certain degree of molecularly undetected patients remains, especially in type 2. This study aims to pinpoint causative variants using different NGS approaches in a cohort of 26 Brazilian probands with possible/probable diagnosis of WS1 (8) or WS2 (18). DNA from the patients was first analyzed by exome sequencing. Seven of these families were submitted to trio analysis. For inconclusive cases, we applied a targeted NGS panel targeting WS/neurocristopathies genes. Causative variants were detected in 20 of the 26 probands analyzed, these being five in PAX3, eight in MITF, two in SOX10, four in EDNRB, and one in ACTG1 (type 2 Baraitser-Winter syndrome, BWS2). In conclusion, in our cohort of patients, the detection rate of the causative variant was 77%, confirming the superior detection power of NGS in genetically heterogeneous diseases.
Full article
(This article belongs to the Special Issue Genetics of Hearing Loss—Volume II)
►▼
Show Figures
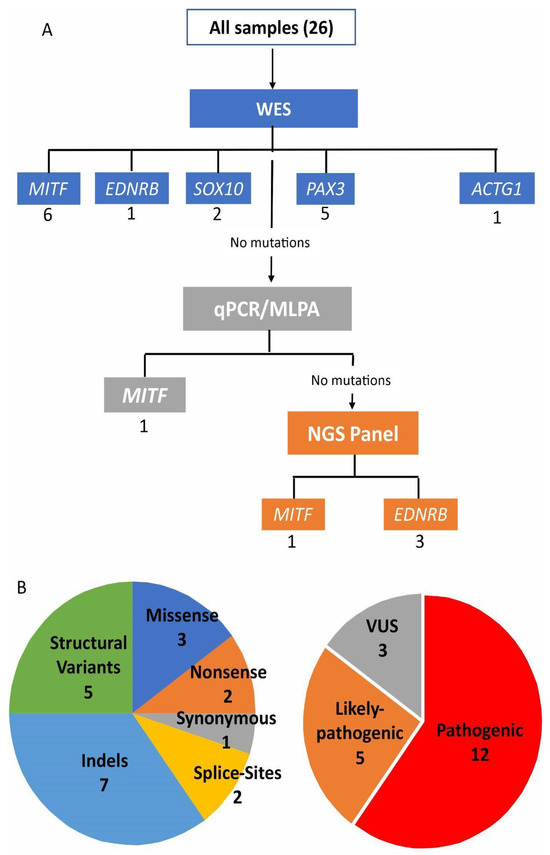
Figure 1
Open AccessCase Report
Osteoneogenesis at the Round Window: A Possible Cause of Cochlear Implant Failure?
Audiol. Res. 2024, 14(1), 1-8; https://doi.org/10.3390/audiolres14010001 - 21 Dec 2023
Abstract
►▼
Show Figures
Surgery for cochlear implant is a traumatic procedure, with inflammatory responses leading to immediate and delayed intracochlear changes, resulting in newly formed fibrous and bony tissue. This newly formed tissue is thought to affect speech perception with cochlear implants and can also play
[...] Read more.
Surgery for cochlear implant is a traumatic procedure, with inflammatory responses leading to immediate and delayed intracochlear changes, resulting in newly formed fibrous and bony tissue. This newly formed tissue is thought to affect speech perception with cochlear implants and can also play a role in causing device malfunctioning and soft failures. We present a case of left cochlear implant explantation and reimplantation in a 15-year-old girl, who experienced deterioration of speech perception and device failure associated with osteoneogenesis of the round window, which could represent a cause of cochlear implant failure. To avoid surgical trauma of the cochlear lateral wall, enlarged round window insertion rather than a cochleostomy, soft surgical techniques, and the application of steroids are all important issues to prevent new tissue formation, although special attention should also be given to the trauma of round window borders.
Full article
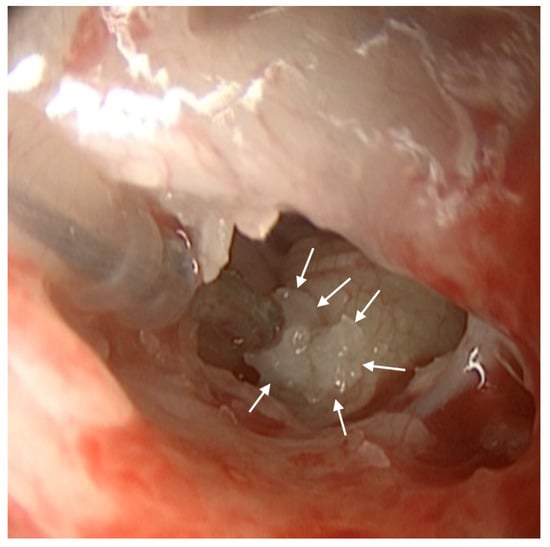
Figure 1
Open AccessCase Report
Which Came First? When Usher Syndrome Type 1 Couples with Neuropsychiatric Disorders
by
, , , , , and
Audiol. Res. 2023, 13(6), 989-995; https://doi.org/10.3390/audiolres13060086 - 11 Dec 2023
Abstract
Usher syndrome (USH) is an autosomal recessive disorder characterized by sensorineural hearing loss (HL), retinopathy, and vestibular areflexia, with variable severity. Although a high prevalence of behavioural and mental disorders in USH patients has been reported, few studies on these psychiatric and psychological
[...] Read more.
Usher syndrome (USH) is an autosomal recessive disorder characterized by sensorineural hearing loss (HL), retinopathy, and vestibular areflexia, with variable severity. Although a high prevalence of behavioural and mental disorders in USH patients has been reported, few studies on these psychiatric and psychological issues have been conducted. This work describes the case of a 16-year-old boy affected by congenital bilateral sensorineural HL, presenting a suddenly altered behaviour concomitant with a decrease in visual acuity. To establish a molecular diagnosis, Whole-Exome Sequencing analysis was performed, detecting a pathogenetic homozygous variant (c. 5985C>A, p.(Tyr1995*)) within the CDH23 gene. CDH23 is a known USH type 1 causative gene, recently associated with schizophrenia-like symptoms and bipolar disorders. To date, no studies have provided evidence of a direct genotype–phenotype correlation between USH patients carrying CDH23 variants and mental/behavioural issues; however, considering the multiple biological functions of CDH23, it can be hypothesised that it could have a pleiotropic effect. Overall, this study highlights the relevance of a continuous clinical evaluation of USH patients, to monitor not only the disease progression, but to early detect any psychological or behavioural alterations, thus allowing a rapid implementation of therapeutic strategies aimed at improving their quality of life and well-being.
Full article
(This article belongs to the Special Issue Genetics of Hearing Loss—Volume II)
►▼
Show Figures
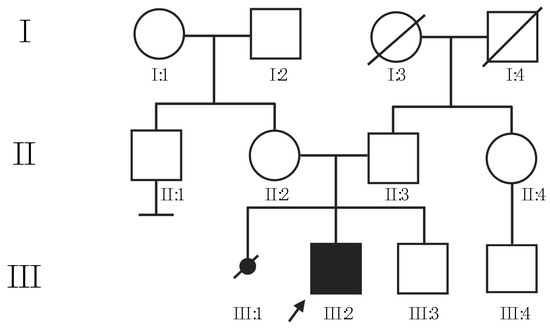
Figure 1
Open AccessArticle
Exploring Electrode Placements to Optimize the Identification and Measurement of Early Auditory Evoked Potentials
Audiol. Res. 2023, 13(6), 978-988; https://doi.org/10.3390/audiolres13060085 - 11 Dec 2023
Abstract
►▼
Show Figures
Cochlear synaptic loss (termed cochlear synaptopathy) has been suggested to contribute to suprathreshold hearing difficulties. However, its existence and putative effects in humans remain inconclusive, largely due to the heterogeneous methods used across studies to indirectly evaluate the health of cochlear synapses. There
[...] Read more.
Cochlear synaptic loss (termed cochlear synaptopathy) has been suggested to contribute to suprathreshold hearing difficulties. However, its existence and putative effects in humans remain inconclusive, largely due to the heterogeneous methods used across studies to indirectly evaluate the health of cochlear synapses. There is a need to standardize proxies of cochlear synaptopathy to appropriately compare and interpret findings across studies. Early auditory evoked potentials (AEPs), including the compound action potential (AP)/Wave I of the auditory brainstem response are a popular proxy, yet remain variable based on technical considerations. This study evaluated one such consideration—electrode array (i.e., montage)—to optimize the use of early AEP waveforms. In 35 young adults, electrocochleography (ECochG) responses were collected using vertical and horizontal montages. Standard ECochG measures and AP/Wave I and Wave II peak-to-trough amplitudes and latencies were compared between montages. Vertical montage recordings consistently produced significantly larger AP/Wave I peak-to-trough amplitudes compared to horizontal recordings. These findings support the use of a vertical electrode montage for optimal recordings of peripheral cochlear nerve activity. As cochlear synaptopathy continues to be explored in humans, the methods highlighted here should be considered in the development of a standardized assessment.
Full article

Figure 1
Open AccessArticle
Evaluation of Cochlear Symptoms in Migraine Patients without Vestibular Migraine and/or Ménière’s Disease
by
, , , , , and
Audiol. Res. 2023, 13(6), 967-977; https://doi.org/10.3390/audiolres13060084 - 06 Dec 2023
Abstract
►▼
Show Figures
Migraine pathogenic pathways may selectively target the cochlea. A qualitative and quantitative analysis of cochlear symptoms in migraine patients without vestibular migraine and/or Méniere’s disease was conducted. We examined 60 consecutive patients with history of cochlear symptoms, including fullness, tinnitus, and hearing loss.
[...] Read more.
Migraine pathogenic pathways may selectively target the cochlea. A qualitative and quantitative analysis of cochlear symptoms in migraine patients without vestibular migraine and/or Méniere’s disease was conducted. We examined 60 consecutive patients with history of cochlear symptoms, including fullness, tinnitus, and hearing loss. Patients were divided into two groups based on migraine history: M (migraine) and nM (no migraine). The incidence of migraine was compared to a homogeneous control group with dysfunctional and inflammatory dysphonia without cochlear symptoms. The type, time of onset, recurrence, bilaterality of symptoms, and hearing threshold were analyzed. The incidence of migraine was significantly higher (p = 0.04) in patients with cochlear symptoms than in the control group. The onset of symptoms is significantly earlier (p < 0.05) in the presence of migraine. The fullness, recurrence, and bilaterality of symptoms are associated with migraine in a statistically significant way (p < 0.05). Pure tone audiometry shows a statistically significant increase in the hearing threshold (500–1000 Hz) in group M. Based on developing findings, cochlear migraine may be considered as a novel clinical entity, like vestibular migraine. It would be the expression, in the absence of vertiginous symptoms, of a selective suffering of the anterior labyrinth by known operating mechanisms of migraine.
Full article

Figure 1
Open AccessFeature PaperReview
Gene Therapy for Inherited Hearing Loss: Updates and Remaining Challenges
by
and
Audiol. Res. 2023, 13(6), 952-966; https://doi.org/10.3390/audiolres13060083 - 04 Dec 2023
Abstract
Hearing loss stands as the most prevalent sensory deficit among humans, posing a significant global health challenge. Projections indicate that by 2050, approximately 10% of the world’s population will grapple with disabling hearing impairment. While approximately half of congenital hearing loss cases have
[...] Read more.
Hearing loss stands as the most prevalent sensory deficit among humans, posing a significant global health challenge. Projections indicate that by 2050, approximately 10% of the world’s population will grapple with disabling hearing impairment. While approximately half of congenital hearing loss cases have a genetic etiology, traditional interventions such as hearing aids and cochlear implants do not completely restore normal hearing. The absence of biological treatment has prompted significant efforts in recent years, with a strong focus on gene therapy to address hereditary hearing loss. Although several studies have exhibited promising recovery from common forms of genetic deafness in mouse models, existing challenges must be overcome to make gene therapy applicable in the near future. Herein, we summarize the primary gene therapy strategies employed over past years, provide an overview of the recent achievements in preclinical studies for genetic hearing loss, and outline the current key obstacles to cochlear gene therapy.
Full article
(This article belongs to the Special Issue Genetics of Hearing Loss—Volume II)
►▼
Show Figures
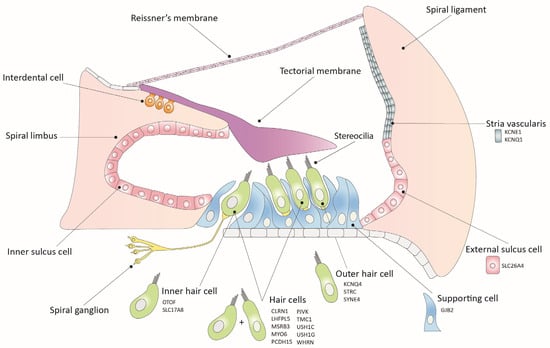
Figure 1
Open AccessArticle
Preceding Benign Paroxysmal Positional Vertigo as a Trigger for Persistent Postural–Perceptual Dizziness: Which Clinical Predictors?
Audiol. Res. 2023, 13(6), 942-951; https://doi.org/10.3390/audiolres13060082 - 01 Dec 2023
Abstract
►▼
Show Figures
Objective: Persistent postural–perceptual dizziness (PPPD) is a syndrome described as secondary, when it is the consequence of an organic disorder (s-PPPD), or primary, when no somatic triggers can be identified. We evaluated a group of patients diagnosed as s-PPPD, with Benign Positional Paroxysmal
[...] Read more.
Objective: Persistent postural–perceptual dizziness (PPPD) is a syndrome described as secondary, when it is the consequence of an organic disorder (s-PPPD), or primary, when no somatic triggers can be identified. We evaluated a group of patients diagnosed as s-PPPD, with Benign Positional Paroxysmal Vertigo (BPPV) as the main somatic trigger, with the aim of identifying the predictive clinical elements of evolution towards PPPD. Study Design: Retrospective case review. Setting: Tertiary referral center. Patients: We evaluated 126 patients diagnosed with PPPD; 54 patients were classified as p-PPPD (43%) and 72 as s-PPPD (57%). Of these, 51 patients had BPPV as a somatic trigger of PPPD, and in this group, we evaluated the prevalence of some clinical features (age, sex, latency between the onset of BPPV and the final diagnosis, recurrence of BPPV and the presence of migraine headache) for comparison with a group of patients who suffered from BPPV without an evolution towards PPPD (control group). Results: In the group with PPPD secondary to BPPV, we found a significantly higher mean age and a longer latency between the onset of BPPV and the final diagnosis compared to the control group. No difference between the two groups was found regarding sex, recurrence rate and the presence of migraine headache. Conclusions: The parameters most involved as potential precipitants of PPPD after BPPV were the age of the patients and a long latency between the onset of BPPV and the final diagnosis; the mean age of the subjects who developed PPPD following BPPV was significantly higher. These findings lead us to emphasize the importance of the early identification and treatment of BPPV, especially in older patients.
Full article

Figure 1
Open AccessEditorial
Robert J. Gorlin: Personal Memory of a Friend and Mentor in Clinical Genetics
Audiol. Res. 2023, 13(6), 939-941; https://doi.org/10.3390/audiolres13060081 - 23 Nov 2023
Abstract
Robert J [...]
Full article
(This article belongs to the Special Issue Genetics of Hearing Loss—Volume II)
►▼
Show Figures

Figure 1
Open AccessCommunication
Does Trauma-Informed Care Have a Place in Audiology? A Review and Practical Suggestions
Audiol. Res. 2023, 13(6), 929-938; https://doi.org/10.3390/audiolres13060080 - 10 Nov 2023
Abstract
►▼
Show Figures
Background. Trauma from adverse childhood experiences (ACEs) and serious traumatic events in adulthood is a significantly prevalent concern for public-health-hearing healthcare professionals. The pediatric and geriatric populations that audiologists often work with have been shown to be at an increased risk of experiencing
[...] Read more.
Background. Trauma from adverse childhood experiences (ACEs) and serious traumatic events in adulthood is a significantly prevalent concern for public-health-hearing healthcare professionals. The pediatric and geriatric populations that audiologists often work with have been shown to be at an increased risk of experiencing traumatic events. Childhood and adult trauma can significantly impact the hearing and vestibular testing and treatment of these patients. Methods. This narrative review article discusses trauma-informed care (TIC) strategies that audiologists can use to recognize and respond to trauma in patients and prevent retraumatizing patients during their encounters in audiology clinics. Conclusions. This article will provide an overview of TIC and direct the reader to resources for their continued learning. Practical guidance on implementing trauma-informed practices in clinical audiology are also provided.
Full article

Figure 1
Open AccessReview
Vestibular Testing—New Physiological Results for the Optimization of Clinical VEMP Stimuli
Audiol. Res. 2023, 13(6), 910-928; https://doi.org/10.3390/audiolres13060079 - 09 Nov 2023
Abstract
Both auditory and vestibular primary afferent neurons can be activated by sound and vibration. This review relates the differences between them to the different receptor/synaptic mechanisms of the two systems, as shown by indicators of peripheral function—cochlear and vestibular compound action potentials (cCAPs
[...] Read more.
Both auditory and vestibular primary afferent neurons can be activated by sound and vibration. This review relates the differences between them to the different receptor/synaptic mechanisms of the two systems, as shown by indicators of peripheral function—cochlear and vestibular compound action potentials (cCAPs and vCAPs)—to click stimulation as recorded in animal studies. Sound- and vibration-sensitive type 1 receptors at the striola of the utricular macula are enveloped by the unique calyx afferent ending, which has three modes of synaptic transmission. Glutamate is the transmitter for both cochlear and vestibular primary afferents; however, blocking glutamate transmission has very little effect on vCAPs but greatly reduces cCAPs. We suggest that the ultrafast non-quantal synaptic mechanism called resistive coupling is the cause of the short latency vestibular afferent responses and related results—failure of transmitter blockade, masking, and temporal precision. This “ultrafast” non-quantal transmission is effectively electrical coupling that is dependent on the membrane potentials of the calyx and the type 1 receptor. The major clinical implication is that decreasing stimulus rise time increases vCAP response, corresponding to the increased VEMP response in human subjects. Short rise times are optimal in human clinical VEMP testing, whereas long rise times are mandatory for audiometric threshold testing.
Full article
(This article belongs to the Special Issue The Vestibular System: Physiology and Testing Methods)
►▼
Show Figures
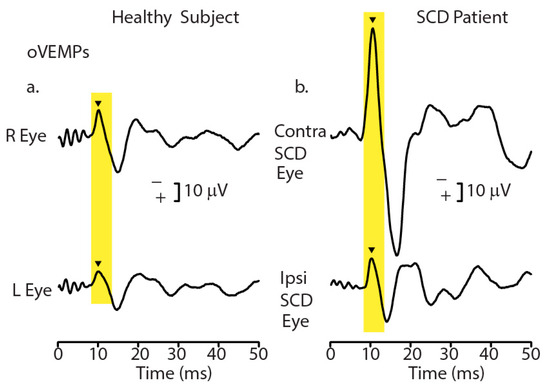
Figure 1
Open AccessArticle
Cartilage Conduction Sounds in Cases of Wearing Different Transducers on a Head and Torso Simulator with a Manipulated Ear Pinna Simulator
Audiol. Res. 2023, 13(6), 898-909; https://doi.org/10.3390/audiolres13060078 - 09 Nov 2023
Abstract
Cartilage conduction is known widely as a third hearing transmission mechanism after the air and bone conduction methods, and transducers dedicated to the production of cartilage conduction sounds have been developed by several Japanese companies. To estimate the acoustic performance of the five
[...] Read more.
Cartilage conduction is known widely as a third hearing transmission mechanism after the air and bone conduction methods, and transducers dedicated to the production of cartilage conduction sounds have been developed by several Japanese companies. To estimate the acoustic performance of the five cartilage conduction transducers selected for this study, both airborne sounds and cartilage conduction sounds were measured. Airborne sounds can be measured using a commercial condenser microphone; however, cartilage conduction sounds are impossible to measure using a conventional head and torso simulator (HATS), because the standard-issue ear pinna simulator cannot reproduce cartilage conduction sounds with the same spectral characteristics as the corresponding sounds measured in humans. Therefore, this study replaced the standard-issue simulator with a developed pinna simulator that can produce similar spectral characteristics to those of humans. The HATS manipulated in this manner realized results demonstrating that transducers that fitted the entrance to the external auditory canal more densely could produce greater cartilage conduction sounds. Among the five transducers under test, the ring-shaped device, which was not much larger than the entrance to the canal, satisfied the spectral requirements.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction—Volume II)
►▼
Show Figures
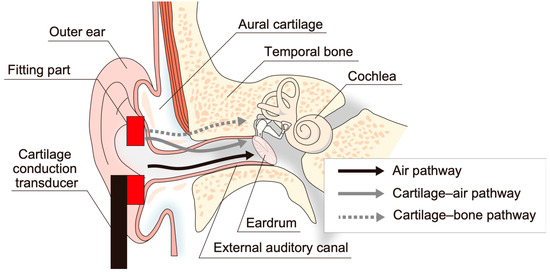
Figure 1
Open AccessSystematic Review
Acute Otitis Media and Facial Paralysis in Children: A Systemic Review and Proposal of an Operative Algorithm
by
, , , and
Audiol. Res. 2023, 13(6), 889-897; https://doi.org/10.3390/audiolres13060077 - 08 Nov 2023
Abstract
►▼
Show Figures
Acute otitis media (AOM) is one of the most common ENT diseases in children. In the antibiotic/post-antibiotic era, facial paralysis is a very rare complication of AOM (0.004–0.005%). Despite the rarity of this complication, it should be known by all physicians for proper
[...] Read more.
Acute otitis media (AOM) is one of the most common ENT diseases in children. In the antibiotic/post-antibiotic era, facial paralysis is a very rare complication of AOM (0.004–0.005%). Despite the rarity of this complication, it should be known by all physicians for proper therapeutic management to avoid serious sequelae. The aim of this review is to provide a management guide based on the current literature. Materials and Methods: Fifteen studies published between 2000 and 2022 were selected, including 120 patients (62 M/58 F) with an average age of 4.96 years old (range = 4 months–16 years; SD: 4.2). The paralysis frequently has a sudden onset and is of a severe grade (medium House–Brackmann (HB) score at onset: 4.68; SD: 0.5); however, it tends to have an almost complete recovery in most patients (88.49% HB 1 at follow-up). Results: Its first-line treatment must be based on the use of antibiotics (beta-lactam antibiotics as penicillins or cephalosporins). Corticosteroids should be used concomitantly for their anti-inflammatory and neuroprotective actions; however, there is no unanimity between authors about their application. Myringotomy, with or without ventilation tube insertion, is indicated in cases where the tympanic membrane is intact. Other kinds of surgery should be performed only in patients who have a worsening of their AOM symptoms or a worsening in HB score even with clinical treatment. Conclusions: The obtained data show that a conservative treatment can be sufficient for complete recovery in most patients, and it is preferred as the first-line therapy. Mastoidectomy should be performed only in patients with acute mastoiditis and without symptom improvement after a conservative approach. There are insufficient data in the current literature to provide clear selection criteria for patients who need to undergo mastoidectomy with facial nerve decompression. The choice of this treatment is based on an individual center expertise. Further studies are needed to clarify the role of corticosteroids and the role of facial nerve decompression in this clinical scenario.
Full article
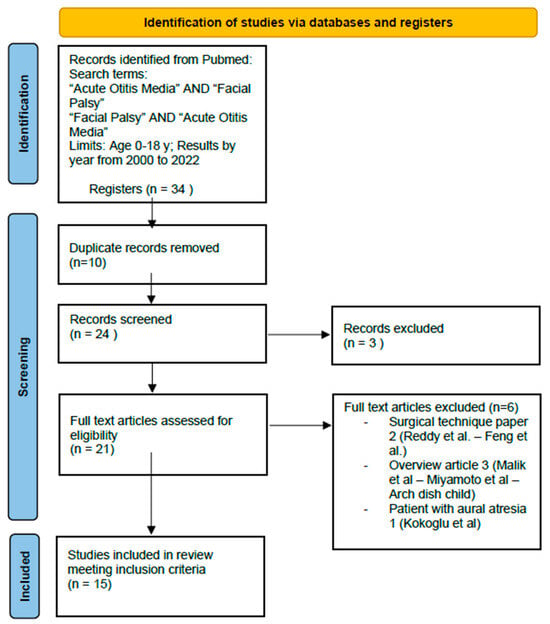
Figure 1
Open AccessArticle
Management of Cartilage Conduction Hearing Aids in Pediatric Patients
by
, , , , , and
Audiol. Res. 2023, 13(6), 871-888; https://doi.org/10.3390/audiolres13060076 - 06 Nov 2023
Abstract
Forty-nine children who started wearing cartilage conduction hearing aids (CC-HAs) before completing elementary school (17 with bilateral hearing loss and 32 with unilateral hearing loss) were followed-up and examined. The wearing and utilization status of the CC-HA and its progress to date were
[...] Read more.
Forty-nine children who started wearing cartilage conduction hearing aids (CC-HAs) before completing elementary school (17 with bilateral hearing loss and 32 with unilateral hearing loss) were followed-up and examined. The wearing and utilization status of the CC-HA and its progress to date were evaluated. In addition, 33 participants who purchased the CC-HAs were interviewed to assess the wearing effect. Eleven of seventeen children with bilateral hearing loss and 25 of 32 children with unilateral hearing loss continued to use the CC-HAs. In terms of wearing effect, a good wearing effect was reported, even by those with unilateral hearing loss. In cases where it was difficult to wear CC-HAs stably with pasting or ear tips, it was possible to fix them stably using commercially available hair bands and eyeglass vines. In two cases, the CC-HAs were worn from infancy. With ingenuity and appropriate educational and medical support, it is possible to wear CC-HAs from infancy.
Full article
(This article belongs to the Special Issue Bone and Cartilage Conduction—Volume II)
►▼
Show Figures
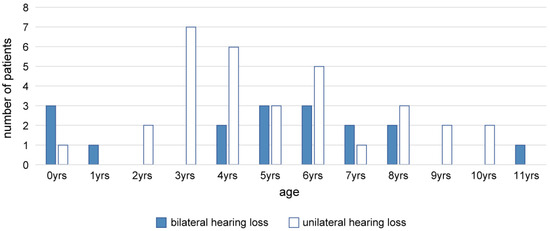
Figure 1
Open AccessArticle
Cross-Cultural Translation and Adaptation of the Consumer Ear Disease Risk Assessment (CEDRA) Questionnaire in Danish
Audiol. Res. 2023, 13(6), 859-870; https://doi.org/10.3390/audiolres13060075 - 02 Nov 2023
Abstract
►▼
Show Figures
This study aimed to cross-culturally translate and adapt the Consumer Ear Disease Risk Assessment (CEDRA) questionnaire into Danish for remote ear, nose, and, throat assessments in adult, first-time hearing aid users when used in conjunction with audiometric measures and visual images of the
[...] Read more.
This study aimed to cross-culturally translate and adapt the Consumer Ear Disease Risk Assessment (CEDRA) questionnaire into Danish for remote ear, nose, and, throat assessments in adult, first-time hearing aid users when used in conjunction with audiometric measures and visual images of the tympanic membrane. Employing field-specific guidelines, the tool underwent a rigorous translation process. This was succeeded by field testing via cognitive debriefing with 30 intendent respondents and a pilot test involving 600 adult, potential first-time hearing aid users from 2020–2022. Test–retest reliability analysis in 113 respondents revealed high consistency and reproducibility, with most items showing Spearman’s correlation coefficients of 0.82 or higher and a Pearson’s correlation of 0.92 for the total score. The tool demonstrated moderate discriminative ability in identifying individuals at high and low risk of complicated hearing loss and targeted ear diseases, supported by an area under the curve of 0.82 on the receiver operating characteristics curve. Our findings suggest that the Danish-translated version of CEDRA is a reliable and effective screening instrument when used with audiometry and tympanometry, warranting further validation in a larger population.
Full article

Figure 1
Open AccessArticle
Episodic Vertigo: A Narrative Review Based on a Single-Center Clinical Experience
Audiol. Res. 2023, 13(6), 845-858; https://doi.org/10.3390/audiolres13060074 - 01 Nov 2023
Abstract
(1) Background: Usually, the majority of patients suffering from vertigo and dizziness can be identified in four major categories: acute spontaneous vertigo, episodic (recurrent) vertigo, recurrent positional vertigo, and chronic imbalance. Our purpose is to retrospectively evaluate the main causes of episodic vertigo
[...] Read more.
(1) Background: Usually, the majority of patients suffering from vertigo and dizziness can be identified in four major categories: acute spontaneous vertigo, episodic (recurrent) vertigo, recurrent positional vertigo, and chronic imbalance. Our purpose is to retrospectively evaluate the main causes of episodic vertigo and to find indications for a reliable clinical suspicion useful for a definitive diagnosis, comparing patients affected by different presenting symptomatology (acute vertigo, recurrent episodic vertigo, and imbalance). (2) Methods: we retrospectively evaluated the clinical records in a population of 249 consecutive patients observed for vertigo in our tertiary referral center in the period 1 January 2019–31 January 2020. On the basis of the reported clinical history, patients were divided into three groups: patients with their first ever attack of vertigo, patients with recurrent vertigo and dizziness, and patients with chronic imbalance. (3) Results: On the basis of the results of the instrumental examination, we arbitrarily divided (for each type of symptoms) the patients in a group with a normal vestibular instrumental examination and a group of patients in which the clinical–instrumental evaluation showed some pathological results; a highly significant difference (p: 0.157) was found between recurrent and acute vertigo and between recurrent vertigo and imbalance. (4) Conclusions: Patients with recurrent vertigo more frequently exhibit a negative otoneurological examination since they are often examined in the intercritical phase. A precise and in-depth research of the patient’s clinical history is the key to suspect or make a diagnosis together with the search for some instrumental or clinical hallmark, especially in cases where the clinical picture does not fully meet the international diagnostic criteria.
Full article
(This article belongs to the Special Issue Episodic Vertigo: Differences, Overlappings, Opinion and Treatment)
►▼
Show Figures
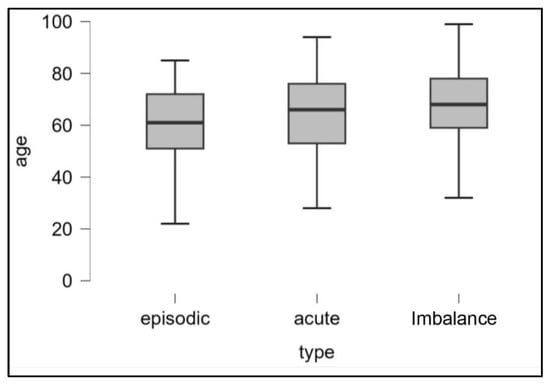
Figure 1

Journal Menu
► ▼ Journal Menu-
- Audiology Research Home
- Aims & Scope
- Editorial Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Topical Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Audiology Research
Genetics of Hearing Loss—Volume II
Guest Editors: Alessandro Martini, Giorgia GirottoDeadline: 29 February 2024
Special Issue in
Audiology Research
Rehabilitation of Hearing Impairment: 2nd Edition
Guest Editor: Sten HellströmDeadline: 30 April 2024
Special Issue in
Audiology Research
The Vestibular System: Physiology and Testing Methods
Guest Editors: Giacinto Asprella Libonati, Herman Kingma, Vito Enrico PettorossiDeadline: 30 June 2024
Topical Collections
Topical Collection in
Audiology Research
Cochlear Implants: Challenges and Opportunities in Hearing Rehabilitation
Collection Editors: Andrea Ciorba, Daniele Borsetto
Topical Collection in
Audiology Research
Translational Audiology
Collection Editor: Agnieszka Szczepek