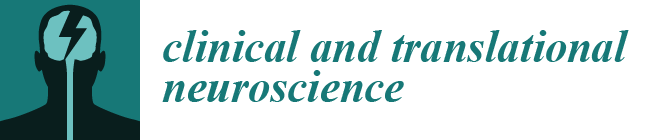Journal Description
Clinical and Translational Neuroscience
Clinical and Translational Neuroscience
is an international, peer-reviewed, open access journal on neuroscience. The journal is owned by the Swiss Federation of Clinical Neuro-Societies and is published quarterly online by MDPI (from Volume 5 Issue 2-2021).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 20.6 days after submission; acceptance to publication is undertaken in 3.5 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Latest Articles
Cellular Stress, Energy Constraints and the Energy Allocation Hypothesis of Sleep
Clin. Transl. Neurosci. 2024, 8(1), 6; https://doi.org/10.3390/ctn8010006 - 10 Jan 2024
Abstract
A growing body of literature demonstrates a critical role for sleep in upregulating diverse biological processes related to protein synthesis, immune function, and cellular housekeeping such as intracellular transport and membrane repair. The energy allocation (EA) hypothesis places sleep in a broader context
[...] Read more.
A growing body of literature demonstrates a critical role for sleep in upregulating diverse biological processes related to protein synthesis, immune function, and cellular housekeeping such as intracellular transport and membrane repair. The energy allocation (EA) hypothesis places sleep in a broader context of resource optimization where sleep–wake partitioning of metabolic operations optimizes resource utilization. The EA hypothesis of sleep carries important implications in health, disease, and homeostatic mechanisms. Specifically, conditions that lead to cellular stress, energy constraints or depression of neuronal activity, such as epilepsy, ischemic stroke or cortical spreading depression, are here proposed to follow similar conserved processes that favor sleep. This review examines the role of local mechanisms, including cytokine release or the accumulation of adenosine, in downregulating wakefulness to favoring sleep, loss of functional connectivity and the upregulation sleep-coupled processes that promote survival.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessReview
The Two-Process Model: Origin of Its Concepts and Their Implications
by
and
Clin. Transl. Neurosci. 2024, 8(1), 5; https://doi.org/10.3390/ctn8010005 - 30 Dec 2023
Abstract
The two-process model of sleep regulation has served as a conceptual framework in the last four decades for understanding sleep physiology. In the 1970s, long-term recordings of sleep in rats were obtained thanks to EEG telemetry. NonREM sleep and REM sleep were found
[...] Read more.
The two-process model of sleep regulation has served as a conceptual framework in the last four decades for understanding sleep physiology. In the 1970s, long-term recordings of sleep in rats were obtained thanks to EEG telemetry. NonREM sleep and REM sleep were found to differ in their time course and response to light-dark protocols. There were indications for their coupling to the circadian system, in particular the light-dark and the dark-light transitions. With the advent of quantitative EEG analysis, slow-wave activity in nonREM sleep was recognized as a sleep-wake-dependent variable. The term “sleep homeostasis” was coined to specify the regulated balance between sleep and waking. The regulatory homeostatic process was designated as “Process S”. In the two-process model, its interaction with the circadian pacemaker “Process C” can account for sleep duration under various experimental protocols. Local, use-dependent slow-wave activity changes were demonstrated in both humans and rats by the selective, unilateral activation of a cortical region prior to sleep. Finding that rest in invertebrates has sleep-like regulatory properties opened a new realm of animal studies. Comparative sleep studies in a broad variety of animal species confirmed the validity of the basic concepts of the two-process model. Recent studies have addressed sleep-related changes of brain temperature as an indicator of brain metabolism; the application of the model to Drosophila; the divergence of cortical and subcortical states; and sleep in an increasing number of species and taxa.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessCorrection
Correction: Schmid et al. SLEEPexpert+: Blending Internet-Based Cognitive Behavioral Therapy for Insomnia with In-Person Psychotherapy—A Feasibility Study in Routine Care. Clin. Transl. Neurosci. 2023, 7, 27
Clin. Transl. Neurosci. 2024, 8(1), 4; https://doi.org/10.3390/ctn8010004 - 29 Dec 2023
Abstract
The Clinical and Translational Neuroscience Editorial Office would like to make the following correction regarding the academic editor listed in this published paper [...]
Full article
Open AccessReview
Sleep and Adolescent Depression
Clin. Transl. Neurosci. 2024, 8(1), 3; https://doi.org/10.3390/ctn8010003 - 22 Dec 2023
Abstract
Adolescence is a pivotal period of development marked by significant physiological and psychological changes, making youth particularly susceptible to mental health challenges, including depression. A growing body of research has highlighted the important role of sleep in the etiology and exacerbation of adolescent
[...] Read more.
Adolescence is a pivotal period of development marked by significant physiological and psychological changes, making youth particularly susceptible to mental health challenges, including depression. A growing body of research has highlighted the important role of sleep in the etiology and exacerbation of adolescent depression. Disruptions in sleep patterns, including insomnia and irregular sleep-wake cycles, are prevalent among depressed adolescents and can exacerbate depressive symptoms. In this review, we examine alterations to sleep behavior and physiology in adolescent depression. Furthermore, we introduce a theoretical model of hypersomnia in adolescent depression. This manuscript explores the intricate relationship between sleep and adolescent depression, with a focus on future directions for research and intervention.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures
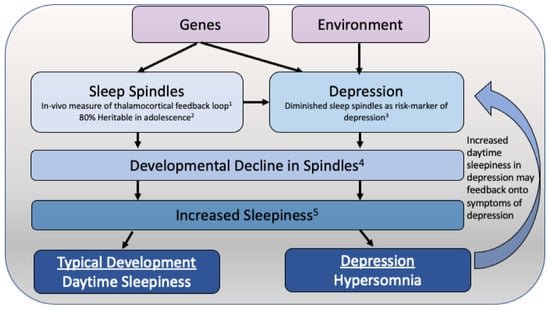
Figure 1
Open AccessFeature PaperArticle
SPHYNCS: The Use of the Swiss Narcolepsy Scale in a New Cohort of Patients with Narcolepsy and Its Borderland and Review of the Literature
by
, , , , , , , , , , , , , , , , and
Clin. Transl. Neurosci. 2024, 8(1), 2; https://doi.org/10.3390/ctn8010002 (registering DOI) - 20 Dec 2023
Abstract
Introduction and aims: Narcolepsy type 1 (NT1) is a central disorder of hypersomnolence (CDH) characterized by excessive daytime sleepiness and cataplexy. The Swiss Narcolepsy Scale (SNS), which includes the updated and short (sSNS) versions, has recently been introduced as a reliable diagnostic tool
[...] Read more.
Introduction and aims: Narcolepsy type 1 (NT1) is a central disorder of hypersomnolence (CDH) characterized by excessive daytime sleepiness and cataplexy. The Swiss Narcolepsy Scale (SNS), which includes the updated and short (sSNS) versions, has recently been introduced as a reliable diagnostic tool for identifying NT1. This study aims to assess the validity of the SNS scales in a new cohort of patients with CDH, while also introducing the French and Italian versions of the SNS and providing a summary of the existing literature on SNS. Materials and methods: The current study is based on the international Swiss Primary Hypersomnolence and Narcolepsy Cohort Study (iSPHYNCS) which aims to identify new biomarkers for CDH. Diagnostic accuracy of the SNS was assessed by calculating sensitivity, specificity, positive predictive value, and negative predictive value. Results: In our population, 108 participants with suspected CDH (including 28 NT1 patients) and 14 healthy controls completed the scale. Original SNS, updated SNS and sSNS scores showed a high sensitivity (86%, 89% and 79%, respectively) and high specificity (96%, 90% and 95%, respectively) for diagnosing NT1 compared to other CDH. The French version was completed by 5 participants, and the Italian version by 8 participants. Regarding previous studies, the SNS has now been assessed in six different populations, involving a total of 1247 subjects (including 326 with narcolepsy with cataplexy/NT1), suggesting high sensitivity (85–100%) and specificity (86–100%) of the SNS for the diagnosis of NT1. Conclusion: The SNS is a simple screening tool validated in seven languages (German, English, French, Italian, Dutch, Turkish and Japanese), demonstrating high sensitivity and specificity for the diagnosis of NT1.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessFeature PaperReview
Is Sleep-Related Eating Disorder (SRED) a NREM Parasomnia or a Heterogenous Disease?
Clin. Transl. Neurosci. 2024, 8(1), 1; https://doi.org/10.3390/ctn8010001 - 19 Dec 2023
Abstract
Sleep-related eating disorder (SRED) is a relatively rare but probably underestimated disorder, where affected patients exhibit nocturnal eating episodes with impaired consciousness and subsequent amnesia. SRED has originally been classified as NREM (non-rapid eye movement) parasomnia, with an obviously high number of concomitant
[...] Read more.
Sleep-related eating disorder (SRED) is a relatively rare but probably underestimated disorder, where affected patients exhibit nocturnal eating episodes with impaired consciousness and subsequent amnesia. SRED has originally been classified as NREM (non-rapid eye movement) parasomnia, with an obviously high number of concomitant sleep disorders. We suggest that SRED may represent a heterogenous disease, based on accumulating data in recent studies. Some SRED patients may be better classified as sleep-related movement disorders with an underlying dopaminergic dysfunction. Hypnotic drugs may play a crucial role in triggering amnestic SRED in both parasomnic and sleep-related movement-disordered SRED.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessReview
Pharmacological Treatments of Sleep–Wake Disorders: Update 2023
Clin. Transl. Neurosci. 2023, 7(4), 42; https://doi.org/10.3390/ctn7040042 - 29 Nov 2023
Abstract
Biological, environmental, behavioral, and social factors can influence sleep and lead to sleep disorders or diseases. Sleep disorders are common, numerous, and heterogeneous in terms of their etiology, pathogenesis, and symptomatology. The management of sleep–wake circadian disorders (SWCDs) includes education on sleep hygiene,
[...] Read more.
Biological, environmental, behavioral, and social factors can influence sleep and lead to sleep disorders or diseases. Sleep disorders are common, numerous, and heterogeneous in terms of their etiology, pathogenesis, and symptomatology. The management of sleep–wake circadian disorders (SWCDs) includes education on sleep hygiene, behavioral strategies, psychotherapy (cognitive behavioral therapy (CBT), particularly), instrument-based treatments (i.e., positive airway pressure therapy, hypoglossal nerve stimulation), and pharmacotherapy. Depending on the disease, therapy varies and is executed sequentially or can be a combination of several forms of therapy. Drugs used for SWCDs include traditional sleep- or wake-promoting agents and chronotherapeutic agents. Recently, novel medications, which more precisely act on specific neurochemical systems (i.e., the orexin system) important for sleep and waking, are also increasingly being used. In this review, the pharmacotherapy of common sleep disorders (insomnia, sleep-related breathing disorder, central disorders of hypersomnolence, circadian rhythm sleep–wake disorders, parasomnias, and sleep-related movement disorders) embedded in the overall therapeutic concept of each disorder is presented. There is also an outlook on possible future pharmacotherapies.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessArticle
Hyperbaric Oxygen in Post-Stroke Patients: A Feasibility Study
Clin. Transl. Neurosci. 2023, 7(4), 41; https://doi.org/10.3390/ctn7040041 - 28 Nov 2023
Abstract
Background: Hyperbaric oxygen therapy (HBOT) has been shown to improve the outcomes of certain stroke patients. Our objective was to assess the feasibility of employing HBOT in daily practice in unselected stroke patients with mild-to-moderate residual post-stroke symptoms, considering their ability to commute
[...] Read more.
Background: Hyperbaric oxygen therapy (HBOT) has been shown to improve the outcomes of certain stroke patients. Our objective was to assess the feasibility of employing HBOT in daily practice in unselected stroke patients with mild-to-moderate residual post-stroke symptoms, considering their ability to commute our center. Methods: This was an exploratory, interventional, prospective monocentric study on post-stroke patients who have completed their in-hospital stroke rehabilitation. We aimed to include 10 participants who were able to complete 40 daily HBOT sessions (2.0 ATA). Effectiveness was assessed using the National Institutes of Health Stroke Score (NIHSS) pre- and post-HBOT. Results: We recruited 13 patients (12 males) with a mean age of 61 years. Three patients dropped out (two never started HBOT and one withdrew after five sessions because of traveling distance). Post-stroke time was 4–251 months. Among the 10 patients completing the HBOT program, 8 improved their NIHSS by a mean of 1,3 (1–4), while 2 patients’ NIHSS remained unchanged. There were no serious adverse events and no side effects. Conclusions: HBOT was shown to be feasible for mobile post-stroke patients who have completed standard rehabilitation. In the absence of major safety concerns, HBOT seems to be an interesting option post-stroke, with the potential to further improve residual stroke severity.
Full article
(This article belongs to the Section Clinical Neurophysiology)
Open AccessReview
Rocking Devices and the Role of Vestibular Stimulation on Sleep—A Systematic Review
Clin. Transl. Neurosci. 2023, 7(4), 40; https://doi.org/10.3390/ctn7040040 - 28 Nov 2023
Abstract
Rocking devices are widely used across different age groups to facilitate sleep. This review discusses the current literature on rocking devices and how passive vestibular stimulation influences sleep architecture, sleep oscillations, and cognitive performance. We included eight studies that conducted research with rocking
[...] Read more.
Rocking devices are widely used across different age groups to facilitate sleep. This review discusses the current literature on rocking devices and how passive vestibular stimulation influences sleep architecture, sleep oscillations, and cognitive performance. We included eight studies that conducted research with rocking devices in humans (7) and mice (1) during daytime naps and/or nighttime sleep, respectively. Overall, vestibular stimulation during sleep induced faster sleep onset, coupled with more N2 in daytime naps or N3 in nighttime sleep. Vestibular stimulation also led to more sleep spindles and better memory consolidation. Optimal stimulation intensity was around 25 cm/s2, and lower intensities led to smaller effects. The findings suggest a sweet spot for vestibular stimulation intensity, promoting deeper sleep at the cost of wakefulness or N1 sleep without compromising REM sleep. While further studies are needed to thoroughly investigate the motion parameters that drive the impact on sleep and cognitive performance, rocking devices may present a promising therapeutic tool for people with disrupted sleep patterns.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessConference Report
Abstracts of the 2023 Joint Annual Meeting of the Swiss Neurological Society and Swiss Society of Neurosurgery Guest Society: Swiss Society of Behavioural Neurology, Kongresshaus Zurich, Switzerland, November 23–24, 2023
Clin. Transl. Neurosci. 2023, 7(4), 39; https://doi.org/10.3390/ctn7040039 - 15 Nov 2023
Abstract
On behalf of the SNS and SSNS, we are pleased to present the abstracts of the Joint Annual Meeting to be held in Zurich, Switzerland, on 23–24 November, 2023. In total, 119 abstracts have been selected: 4 abstracts for the Plenary Sessions, 12
[...] Read more.
On behalf of the SNS and SSNS, we are pleased to present the abstracts of the Joint Annual Meeting to be held in Zurich, Switzerland, on 23–24 November, 2023. In total, 119 abstracts have been selected: 4 abstracts for the Plenary Sessions, 12 abstracts for Free Communications, 18 abstracts for Poster flash presentations, 6 abstracts for the SAYN GemSession, and 79 abstracts as ePosters. We congratulate all the presenters on their research work and contributions.
Full article
Open AccessProject Report
The Swiss Brain Health Plan 2023–2033
by
, , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , , and add
Show full author list
remove
Hide full author list
Clin. Transl. Neurosci. 2023, 7(4), 38; https://doi.org/10.3390/ctn7040038 - 13 Nov 2023
Abstract
►▼
Show Figures
The brain and its health are essential for our (physical mental, social, and spiritual) wellbeing, for being able to realize our potential as individuals, and also for a fair, well-functioning, and productive society. However, today the world is facing a healthcare crisis related
[...] Read more.
The brain and its health are essential for our (physical mental, social, and spiritual) wellbeing, for being able to realize our potential as individuals, and also for a fair, well-functioning, and productive society. However, today the world is facing a healthcare crisis related to the very high (and increasing) burden of brain disorders. As a response to this crisis, the “Swiss Brain Health Plan” (SBHP) was conceptualized in the context of other initiatives launched to value, promote, and protect brain health over the entire life course. In the first section of this position paper, the following fundamental considerations of the SBHP are discussed: (1) the high (and increasing) burden of brain disorders in terms of prevalence (>50% of the population suffers from a brain disorder), disability, mortality, and costs; (2) the prevention of brain disorders; (3) the operational definition of brain health; (4) determinants of brain health; (5) international initiatives to promote brain (including mental) health including the World Health Organization (WHO) intersectorial global action plan on epilepsy and other neurological disorders (NDs) (IGAP) and the WHO comprehensive mental health action plan. In the second section of the paper, the five strategic objectives of the SBHP, which has the vision of promoting brain health for all across the entire life course, are presented: (1) to raise awareness; (2) strengthen cross-disciplinary and interprofessional training/educational programs for healthcare professionals; (3) foster research on brain health determinants and individualized prevention of brain disorders; (4) prioritize a holistic (non-disease-specific), integrated, person-centered public health approach to promote brain health and prevent brain disorders through collaborations across scientific, health care, commercial, societal and governmental stakeholders and insurance providers; (5) support, empower, and engage patients, caregivers, and patient organizations, and reduce the stigma and discrimination related to brain disorders. In the third section of the paper, the first (2024) steps in the implementation of the SHBP, which will be officially launched in Zurich on 22 November 2023, are presented: (1) a definition of the overall organization, governance, specific targets, and action areas of the SBHP; (2) the patronage and/or co-organization of events on such specific topics as brain research (Lausanne), dementia (Geneva), stroke (Basel), neurohumanities (Bellinzona), sleep (Lugano), and psychiatry (Zurich); (3) the conduction of a new study on the global burden of brain disorders in Switzerland; (4) the launching of an international Certificate of Advanced Studies (CAS) on Brain Health at the University of Bern. In the fourth section of the paper, there is a concise executive summary of the SBHP.
Full article

Figure 1
Open AccessReview
The Past and Future of Psychiatric Sleep Research
Clin. Transl. Neurosci. 2023, 7(4), 37; https://doi.org/10.3390/ctn7040037 - 08 Nov 2023
Abstract
Sleep studies in psychiatric disorders date back to the first half of the 20th century. So far, success in establishing disease-specific sleep-related biomarkers has been quite limited. This is particularly obvious regarding insomnia, where there is no reliable correlation between subjective complaints and
[...] Read more.
Sleep studies in psychiatric disorders date back to the first half of the 20th century. So far, success in establishing disease-specific sleep-related biomarkers has been quite limited. This is particularly obvious regarding insomnia, where there is no reliable correlation between subjective complaints and physiological measures of sleep. Finally, it must be acknowledged that the physiology of sleep and wakefulness and their subjective perception are essentially independent dimensions. Still, however, these dimensions are mixed up in clinical practice and research. This creates confusion, can be harmful for patients, and is identified as a major obstacle for successful psychiatric sleep research. It is proposed here that future sleep research should treat physiological sleep as a variable in psychiatric disorders which, independently of patient perception, has a transdiagnostic value, as was already proposed a decade ago by the Research Domain Criteria.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessReview
Thalamic Stroke: An Opportunity to Study the Brain Mechanisms of Sleep–Wake and Cognition
Clin. Transl. Neurosci. 2023, 7(4), 36; https://doi.org/10.3390/ctn7040036 - 31 Oct 2023
Abstract
The thalamus, and its projections to the cerebral cortex, are crucial for regulating sleep rhythms, such as sleep spindles, and for maintaining arousal and sleep homeostasis. Moreover, they play a significant role in memory, executive functioning, and attention. Altered thalamocortical circuitry caused by
[...] Read more.
The thalamus, and its projections to the cerebral cortex, are crucial for regulating sleep rhythms, such as sleep spindles, and for maintaining arousal and sleep homeostasis. Moreover, they play a significant role in memory, executive functioning, and attention. Altered thalamocortical circuitry caused by vascular lesions affects sleep–wake architecture and may contribute to cognitive deficits observed in thalamic stroke patients. This review summarizes the biology of the thalamus and current knowledge regarding the impact of thalamic circuitry on sleep regulation and cognition, drawing from clinical and pre-clinical studies. Furthermore, deep brain stimulation and transcranial magnetic stimulation are discussed as possible therapeutic approaches targeting thalamic circuits. Understanding the role of the thalamus in sleep and cognition opens new avenues for developing novel therapeutic strategies to improve sleep and cognitive functions in affected individuals.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures
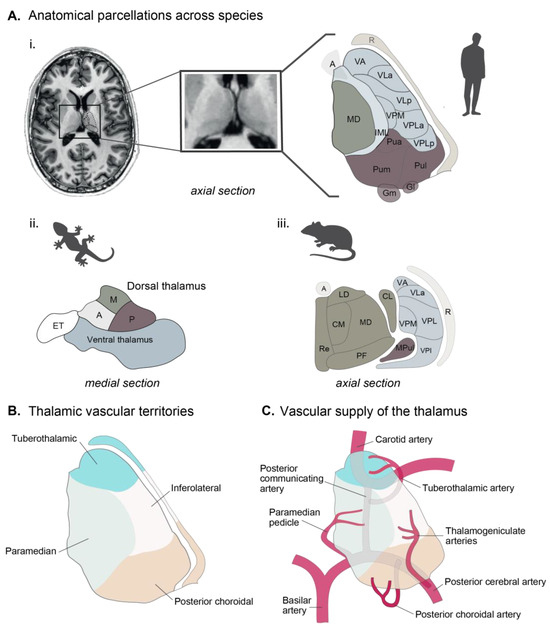
Figure 1
Open AccessArticle
The Neuropsychological and Emotional Profile of Adults with Parasomnia: A Case Series
by
, , , , , , and
Clin. Transl. Neurosci. 2023, 7(4), 35; https://doi.org/10.3390/ctn7040035 - 29 Oct 2023
Abstract
Although parasomnias are nocturnal phenomena occurring during sleep or during arousals from sleep, there is increasing evidence that they are associated with daytime dysfunction as well. However, systematic studies in this field are scarce. The aim of the current case series was to
[...] Read more.
Although parasomnias are nocturnal phenomena occurring during sleep or during arousals from sleep, there is increasing evidence that they are associated with daytime dysfunction as well. However, systematic studies in this field are scarce. The aim of the current case series was to investigate the sleep–wake, neuropsychological and emotional profiles of patients with parasomnias. Thirty patients with parasomnia (13 NREM, 17 REM) and 30 healthy subjects matched for age, sex and educational status were included. All participants underwent comprehensive neuropsychological, cognitive and behavioral evaluation. We found that parasomnia patients scored higher in all neuropsychological, emotional, sleep–wake and quality of life scales compared to healthy subjects. The presence of a parasomnia was associated with major impact on daytime functioning across several domains with increased levels of fatigue (FSS > 4) in 56%, sleepiness (ESS > 10) in 47%, depressive symptoms (BDI > 20) in 17%, anxiety (PSWQ > 52) in 17%, anger expression out (STAXI A > 16) in 27% and anger expression in (STAXI B > 16) in 23%, as well as a reduced average quality of life score (RAND derived from SF-36). Sleep–wake disturbances were significantly correlated with QoL scores. In the intergroup analysis between REM/NREM, we found that the REM group had worse cognitive performance and lower levels of fatigue/energy compared to NREM patients. These findings suggest that parasomnia is associated with difficulties in several aspects of daytime functioning (cognitive, affective/emotional and physical) and, therefore, parasomnia diagnostic workup should not be limited only to nocturnal phenomena.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessArticle
Activity of Corrugator Muscle with Pressure Pain Stimulation in Healthy People
Clin. Transl. Neurosci. 2023, 7(4), 34; https://doi.org/10.3390/ctn7040034 - 27 Oct 2023
Abstract
►▼
Show Figures
Corrugator muscle activity with pressure pain stimulation has not yet been studied. We recorded corrugator muscle activity at rest and before, during and after pressure pain stimulation to the shoulder three times each in 14 healthy adults (20.0 ± 2.1 years of age
[...] Read more.
Corrugator muscle activity with pressure pain stimulation has not yet been studied. We recorded corrugator muscle activity at rest and before, during and after pressure pain stimulation to the shoulder three times each in 14 healthy adults (20.0 ± 2.1 years of age (mean ± SD)) without pain using surface electromyography. Corrugator muscle activity with pressure pain and the relationships between corrugator muscle activity and pressure pain or unpleasantness intensity on a visual analogue scale measured three times were examined. The corrugator muscle activity during pressure pain stimulation was significantly higher than that before (p < 0.001) and after (p = 0.019) stimulation. There were significant differences among the three measurements examining reproducibility in pain (p = 0.037) and unpleasantness (p = 0.014) but not among corrugator muscle activities before (p = 0.526), during (p = 0.145) and after (p = 0.109) stimulation. Significant correlations were revealed for corrugator muscle activity vs. pain (ρ = 0.465, p = 0.002) and corrugator muscle activity vs. unpleasantness (ρ = 0.558, p < 0.001). Pressure pain increased corrugator muscle activity with reproducibility and correlated with subjective pain assessments, which indicates the utility of corrugator muscle activity as an objective indication of pain assessment.
Full article
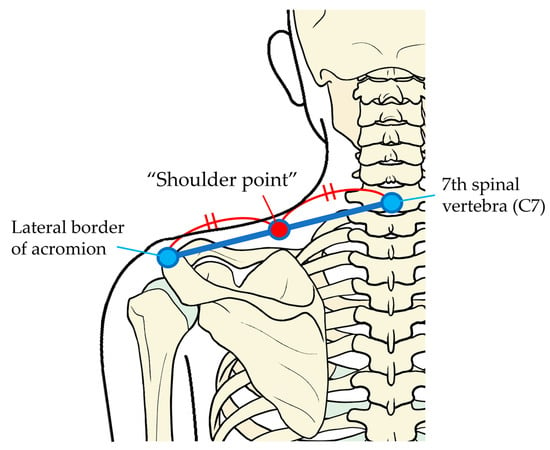
Figure 1
Open AccessArticle
The Sleep of Shift Workers in a UK Financial Organisation and Associations with Mental, Physical, Social and Cognitive Health
Clin. Transl. Neurosci. 2023, 7(4), 33; https://doi.org/10.3390/ctn7040033 - 23 Oct 2023
Abstract
Shift workers are vulnerable to circadian misalignment, sleep disturbance and increased risk of impaired health. Studies concerning the sleep and health of individuals working shifts in the financial sector are lacking. We investigated sleep quality, sleep duration and associations with health in a
[...] Read more.
Shift workers are vulnerable to circadian misalignment, sleep disturbance and increased risk of impaired health. Studies concerning the sleep and health of individuals working shifts in the financial sector are lacking. We investigated sleep quality, sleep duration and associations with health in a UK financial organisation. Employees (n = 178; 61% male) completed an online survey comprising the SSI, PSQI, GAD-7, PHQ-9, WAFCS, EMQ-R and BMI. Three-quarters of employees reported poor sleep quality. Poorer sleep quality and shorter sleep duration were both associated with greater anxiety and depression symptoms. However, sleep quality demonstrated greater explained variance with symptom severity (anxiety: Rs2 difference = 13.2%; depression: Rs2 difference = 21.8%). Poorer sleep quality was associated with higher BMI, greater work-to-family conflict and poorer everyday memory (rs = 0.26–0.29), while shorter sleep duration was only significantly associated with higher BMI. Sleep quality did not differ depending on the nightshift type (“permanent”/“other”). Sleep achieved was shorter than perceived sleep-need for all consecutive shift types—especially night shifts (40 min–1 h 24 min). This preliminary study suggests that sleep quality, and to a lesser extent sleep duration, are associated with a range of health outcomes for shift workers within the financial sector, highlighting the need to increase organisational awareness of the importance of sleep for employee health.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessArticle
Four New Cases of Progressive Ataxia and Palatal Tremor (PAPT) and a Literature Review
Clin. Transl. Neurosci. 2023, 7(4), 32; https://doi.org/10.3390/ctn7040032 - 13 Oct 2023
Abstract
►▼
Show Figures
PAPT syndrome is a rare neurologic disorder characterized by progressive ataxia and palatal tremor (rhythmic movements of the soft palate). The first large study of PAPT patients was published in 2004, included a total of 28 sporadic PAPT cases, and suggested a neurodegenerative
[...] Read more.
PAPT syndrome is a rare neurologic disorder characterized by progressive ataxia and palatal tremor (rhythmic movements of the soft palate). The first large study of PAPT patients was published in 2004, included a total of 28 sporadic PAPT cases, and suggested a neurodegenerative origin. In the last several years, case reports and small case series followed, underlining the heterogeneity of the clinical picture and underlying aetiology (including neurodegenerative, vascular, infectious/autoimmune, and genetic). As a contribution to the literature, we report on four new patients with PAPT syndrome from Bern. Our study highlights the diverse clinical presentation (pyramidal, extrapyramidal, bulbar, cognitive, psychiatric symptoms, and autonomic features), summarizes the known literature, and extends it by findings on sleep studies (obstructive/central sleep apnoea, sleep disturbance). Possible aetiologies and management aspects are discussed in light of the current literature.
Full article
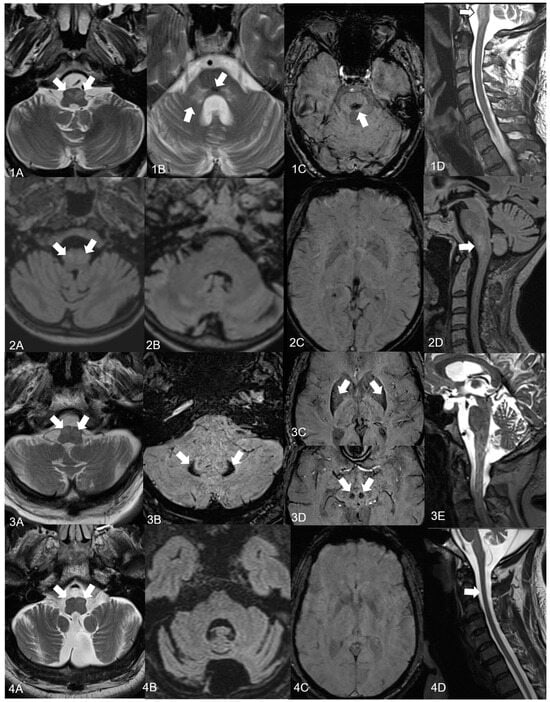
Figure 1
Open AccessCommunication
The Swiss Narcolepsy Network (SNaNe)
Clin. Transl. Neurosci. 2023, 7(4), 31; https://doi.org/10.3390/ctn7040031 - 13 Oct 2023
Abstract
The Swiss Narcolepsy Network (SNaNe) was founded in 2017 as a non-profit organization with the vision of improving the care of patients with narcolepsy, central disorders of hypersomnolence (CDH), and rare sleep disorders. The SNaNe aims at maximizing the speed of diagnosis, minimizing
[...] Read more.
The Swiss Narcolepsy Network (SNaNe) was founded in 2017 as a non-profit organization with the vision of improving the care of patients with narcolepsy, central disorders of hypersomnolence (CDH), and rare sleep disorders. The SNaNe aims at maximizing the speed of diagnosis, minimizing difficulties stemming from the rare nature of these conditions, and providing patients with optimum health care throughout the course of their disease. In addition, the SNaNe promotes education, awareness, and research on CDH and rare sleep disorders. The article reports the current structure, organization, and the following main activities of the SNaNe: (1) the discussion of complex patient cases; (2) the organization of the Swiss Narcolepsy Days; (3) the coordination of multicenter research projects (e.g., SPHYNCS and iSPHYNCS studies); (4) the establishment of an anonymous Swiss registry for CDH patients (SNaNe Data Registry); (5) the collaboration with the national patients’ organization (SNAG); and (6) the collaboration with other national and international scientific, professional, and patients’ (eNAP) organizations.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessReview
The Psychoneurobiology of Insomnia: Hyperarousal and REM Sleep Instability
Clin. Transl. Neurosci. 2023, 7(4), 30; https://doi.org/10.3390/ctn7040030 - 28 Sep 2023
Cited by 1
Abstract
Chronic insomnia (insomnia disorder—ID) afflicts up to 10% of the adult population, increases with age and affects more women than men. ID is associated with significant daytime impairments and an increased risk for developing major somatic and mental disorders, especially depression and anxiety
[...] Read more.
Chronic insomnia (insomnia disorder—ID) afflicts up to 10% of the adult population, increases with age and affects more women than men. ID is associated with significant daytime impairments and an increased risk for developing major somatic and mental disorders, especially depression and anxiety disorders. Almost all insomnia models assume persistent hyperarousal on cognitive, emotional, cortical and physiological levels as a central pathophysiological component. The marked discrepancy between only minor objective alterations in polysomnographic parameters of sleep continuity and the profound subjective impairment in patients with insomnia is still puzzling. We and others have proposed that alterations in the microstructure of sleep, especially in REM sleep (REM sleep instability), may explain this discrepancy and be at the core of the experience of fragmented and poor sleep in ID. The REM sleep instability concept is based on evidence showing REM time to be related to subjective wake time in insomnia as well as increased micro- and macro-arousals during REM sleep in insomnia patients compared to good-sleeper controls. Our own work showed that ID patients awoken from REM sleep more frequently reported the perception of having been awake than good sleepers as well as having had more negative ideations. The continuous measurement of event-related potentials throughout the whole night demonstrated reduced P2 amplitudes specifically during phasic REM sleep in insomnia, which points to a mismatch negativity in ID reflecting automatic change detection in the auditory system and a concomitant orienting response. REM sleep represents the most highly aroused brain state during sleep and thus might be particularly prone to fragmentation in individuals with persistent hyperarousal, resulting in a more conscious-like wake experience reflecting pre-sleep concerns of patients with ID, i.e., worries about poor sleep and its consequences, thus leading to the subjective over-estimation of nocturnal waking time and the experience of disrupted and non-restorative sleep. Chronic REM sleep instability might also lead to a dysfunction in a ventral emotional neural network, including limbic and paralimbic areas activated during REM sleep. Along with a postulated weakened functioning in a dorsal executive neural network, including frontal and prefrontal areas, this might contribute to emotional and cognitive alterations and an elevated risk of developing depression and anxiety.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessArticle
The Good Clinical Outcome for Patients with Acute Ischemic Stroke Treated with Mechanical Thrombectomy—Does Time Still Matter?
Clin. Transl. Neurosci. 2023, 7(3), 29; https://doi.org/10.3390/ctn7030029 - 20 Sep 2023
Abstract
The primary target was an investigation of the factors predicting a good clinical outcome of patients with acute ischemic stroke after treatment with mechanical thrombectomy. Additionally, we compared the treatment results in known and unknown symptom onset time groups. We retrospectively analyzed the
[...] Read more.
The primary target was an investigation of the factors predicting a good clinical outcome of patients with acute ischemic stroke after treatment with mechanical thrombectomy. Additionally, we compared the treatment results in known and unknown symptom onset time groups. We retrospectively analyzed the data from 2012 to 2020 and divided 240 patients into the known and unknown symptom onset time groups. We looked for the variables predicting a good clinical outcome (NIHSS 0–4 at discharge) in both groups. In both groups, there was no statistically significant difference in good clinical outcomes (43% in the known symptom onset time group vs. 33.3% in the unknown symptom onset time group, p = 0.203). Factors predicting a good clinical outcome in both groups were lower NIHSS scores at admission, the presentation of pial arterial collaterals on admission CT angiography, and bridging intravenous thrombolysis. In the known symptom onset time group, lower age was also a factor predicting good outcome. Our clinical results of treatment by using mechanical thrombectomy were comparable in the known and unknown symptom onset time groups.
Full article
(This article belongs to the Section Endovascular Neurointervention)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics