Journal Description
Gastrointestinal Disorders
Gastrointestinal Disorders
is an international, open access, peer-reviewed journal on gastroenterology, published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions; authors retain copyright.
- High Visibility: indexed within Scopus, ESCI (Web of Science), FSTA, and other databases.
- Journal Rank: CiteScore - Q2 (Immunology and Microbiology (miscellaneous))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 21.3 days after submission; acceptance to publication is undertaken in 5.2 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Reliable service: rigorous peer review and professional production.
Impact Factor:
0.7 (2022)
Latest Articles
Endoscopic Management of Gastric Disruptions
Gastrointest. Disord. 2024, 6(1), 131-142; https://doi.org/10.3390/gidisord6010009 - 11 Jan 2024
Abstract
►
Show Figures
Gastric perforations and leaks are significant complications that can arise from various gastrointestinal disorders and surgical interventions. Over the past decade, endoscopic techniques have emerged as an effective method for managing these conditions. Furthermore, as endoscopic resection techniques have grown in popularity, the
[...] Read more.
Gastric perforations and leaks are significant complications that can arise from various gastrointestinal disorders and surgical interventions. Over the past decade, endoscopic techniques have emerged as an effective method for managing these conditions. Furthermore, as endoscopic resection techniques have grown in popularity, the risk of acute and delayed perforations has also grown. This review aims to provide an in-depth analysis of the endoscopic management strategies employed in the management of gastric perforations and leaks. We will discuss the etiology, diagnostic modalities, and various endoscopic techniques utilized, as well as emerging trends in endoscopic management. Our attempt in writing this review paper is to educate and guide clinicians in making informed decisions when faced with gastric perforations and leaks.
Full article
Open AccessSystematic Review
Probiotic Interventions in Coeliac Disease: A Systematic Review with a Focus on Cardiovascular Risk
by
, , , , and
Gastrointest. Disord. 2024, 6(1), 114-130; https://doi.org/10.3390/gidisord6010008 - 10 Jan 2024
Abstract
►▼
Show Figures
People with coeliac disease (CD) have a higher risk of developing cardiovascular disease (CVD), potentially due to inflammation. Probiotics can influence CVD risk through several mechanisms including modifying inflammation. We performed a systematic review of probiotic interventions in people with CD. In total,
[...] Read more.
People with coeliac disease (CD) have a higher risk of developing cardiovascular disease (CVD), potentially due to inflammation. Probiotics can influence CVD risk through several mechanisms including modifying inflammation. We performed a systematic review of probiotic interventions in people with CD. In total, 4 databases were systematically searched for studies published up to March 2023. All outcomes, inclusive of any cardiovascular risk factors, were collated and reported. We screened 8084 articles and 11 publications reporting on 7 RCTs and 2 non-RCTs met the inclusion criteria for qualitative analysis. In total, 1 RCT and both non-RCTs were considered to have a high risk of bias. There was large heterogeneity between the studies and adherence to a gluten-free diet was only measured in two studies. No specific outcomes related to cardiovascular risk were reported. Two studies reported a significant reduction on serum TNF-α in children over time after probiotic supplementation. One study reported no significant change in intestinal permeability over a 3-week intervention. Currently there is insufficient evidence to advocate a positive impact of probiotics on inflammation in CD, due, in part, to the limited data on adherence to the gluten-free diet and active disease.
Full article
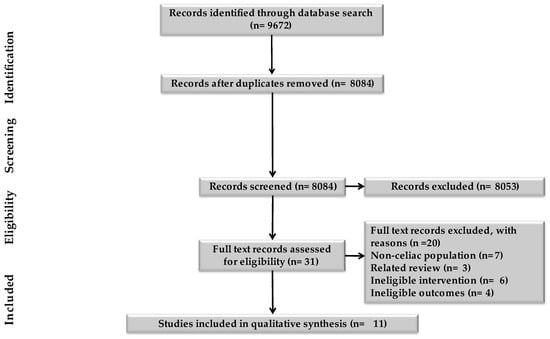
Figure 1
Open AccessArticle
In the Driving Seat with High-Resolution Ano-Rectal Manometry
Gastrointest. Disord. 2024, 6(1), 103-113; https://doi.org/10.3390/gidisord6010007 - 10 Jan 2024
Abstract
►▼
Show Figures
Introduction: High-resolution ano-rectal manometry (HRAM), part of the investigative process to diagnose disorders of recto-anal co-ordination, is currently performed in the left-lateral position (LLP). This may seem unnatural for patients and recent data suggest that the seated, squatted position (SP) may improve rectal
[...] Read more.
Introduction: High-resolution ano-rectal manometry (HRAM), part of the investigative process to diagnose disorders of recto-anal co-ordination, is currently performed in the left-lateral position (LLP). This may seem unnatural for patients and recent data suggest that the seated, squatted position (SP) may improve rectal drive and recto-anal pressure gradients, raising the question as to whether defaecatory dyssenergia (DD) is over-diagnosed when the test is carried out in the LLP. Aim/method: A single centre study was carried out in patients with faecal incontinence and/or constipation to evaluate the effect of SP versus LLP on HRAM analysis and resultant manometric diagnosis of DD. Positioning was consecutive and the order was randomised for each patient. The HRAM protocol was carried out in accordance with the manufacturer’s guidelines (Manoscan). Data analysis and interpretation were blinded with a consensus reached for each test position. Data (mean ± SEM) were analysed using an unpaired t-test and Chi-square test. Results: In total, 40 patients completed the study, including 33 females with a median age of 56 (IQR 48–63). The mean rectal drive was significantly higher in the SP vs. LLP (82.6 ± 5.3 mmHg vs. 44.1 ± 3.9 mmHg, respectively, p < 0.0001). No difference in the anal sphincter relaxation pressure (66.7 ± 5.7 mmHg vs. 70.9 ± 5.5 mmHg, p = 0.9535) was detected. The manometric diagnoses of abnormal ano-rectal co-ordination were significantly higher in the LLP, when p = 0.013. Patients reported a significant preference for the seated position, when p = 0.0001. Conclusion: These data show that HRAM in the seated position improves rectal drive, which reduces manometric diagnoses of abnormal ano-rectal coordination. These findings may have important implications for practice and may inform future guidelines.
Full article
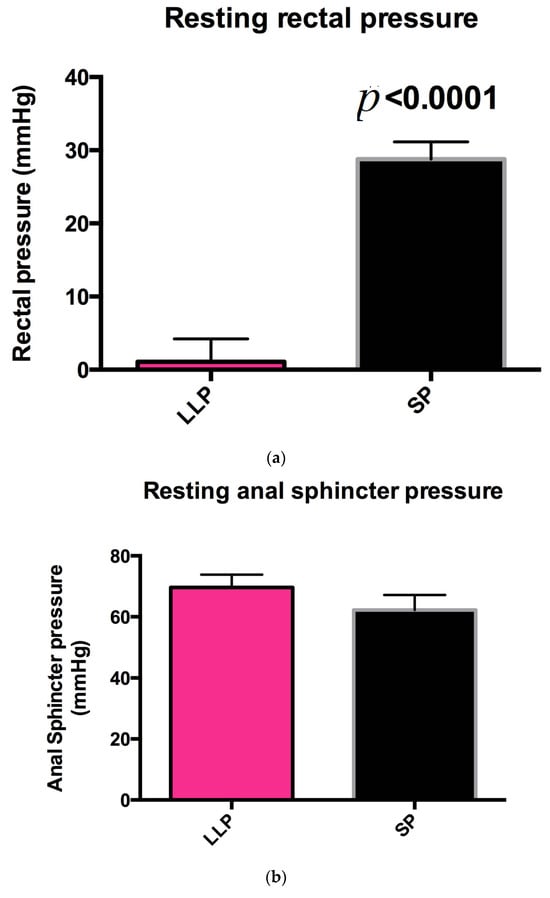
Figure 1
Open AccessSystematic Review
The Diagnostic Accuracy of Abdominal X-ray in Childhood Constipation: A Systematic Review of the Literature
Gastrointest. Disord. 2024, 6(1), 94-102; https://doi.org/10.3390/gidisord6010006 - 09 Jan 2024
Abstract
Background: Previous systematic reviews have found insufficient and conflicting evidence for an association between the clinical and radiographic diagnosis of functional constipation. Abdominal X-ray is frequently used for the diagnosis of functional constipation in clinical practice. The objective of this study was to
[...] Read more.
Background: Previous systematic reviews have found insufficient and conflicting evidence for an association between the clinical and radiographic diagnosis of functional constipation. Abdominal X-ray is frequently used for the diagnosis of functional constipation in clinical practice. The objective of this study was to evaluate the diagnostic accuracy of abdominal X-ray for the evaluation of functional constipation in children. Results: Three studies were included in the final qualitative analysis. They were heterogeneous in their study design, definition of constipation, and radiologic parameters used to evaluate the abdominal X-rays. Sensitivities ranged from 73–92%, specificities ranged from 26–92%, and diagnostic accuracies ranged from 78–90%. Methods: This study involved a systematic review of English literature published between 2012 and 2022 covering children 2–18 years of age with a diagnosis of functional constipation in whom abdominal X-ray was performed. The databases searched include Medline, Embase, and Scopus. Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) and Quality Assessment of Diagnostic Accuracy Studies 2 (QUADAS-2) guidelines were followed. PROSPERO ID: CRD42022301833. Conclusions: There is insufficient evidence to support the use of abdominal X-ray as part of the diagnostic workup of functional constipation. More methodologically rigorous studies are needed to determine the utility of abdominal X-ray in the evaluation of functional constipation. The diagnosis of functional constipation should be based on history and clinical findings.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
►▼
Show Figures
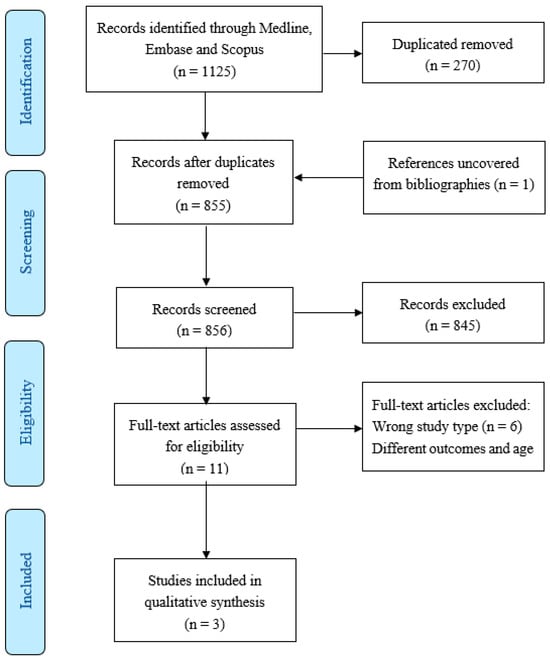
Figure 1
Open AccessReview
Viral Liver Disease and Intestinal Gut–Liver Axis
Gastrointest. Disord. 2024, 6(1), 64-93; https://doi.org/10.3390/gidisord6010005 - 08 Jan 2024
Abstract
The intestinal microbiota is closely related to liver diseases via the intestinal barrier and bile secretion to the gut. Impairment of the barrier can translocate microbes or their components to the liver where they can contribute to liver damage and fibrosis. The components
[...] Read more.
The intestinal microbiota is closely related to liver diseases via the intestinal barrier and bile secretion to the gut. Impairment of the barrier can translocate microbes or their components to the liver where they can contribute to liver damage and fibrosis. The components of the barrier are discussed in this review along with the other elements of the so-called gut–liver axis. This bidirectional relation has been widely studied in alcoholic and non-alcoholic liver disease. However, the involvement of microbiota in the pathogenesis and treatment of viral liver diseases have not been extensively studied, and controversial data have been published. Therefore, we reviewed data regarding the integrity and function of the intestinal barrier and the changes of the intestinal microbioma that contribute to progression of Hepatitis B (HBV) and Hepatitis C (HCV) infection. Their consequences, such as cirrhosis and hepatic encephalopathy, were also discussed in connection with therapeutic interventions such as the effects of antiviral eradication and the use of probiotics that may influence the outcome of liver disease. Profound alterations of the microbioma with significant reduction in microbial diversity and changes in the abundance of both beneficial and pathogenic bacteria were found.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
►▼
Show Figures
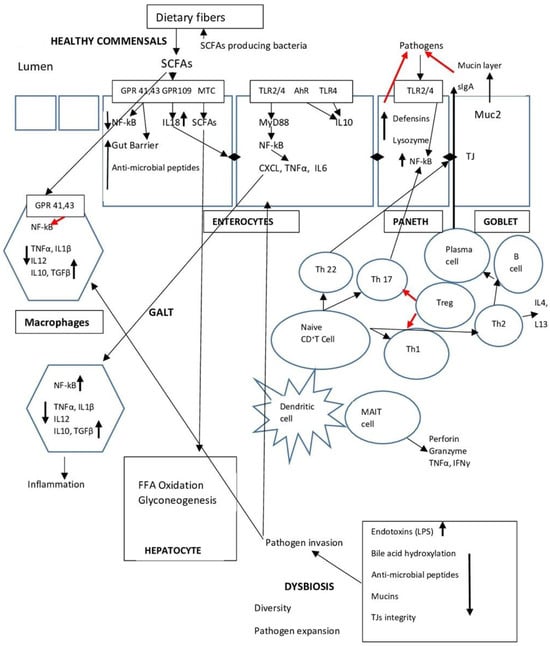
Figure 1
Open AccessArticle
Insights into Personal Perceptions and Experiences of Colonoscopy after Positive FIT in the Flemish Colorectal Cancer Screening Program
by
and
Gastrointest. Disord. 2024, 6(1), 49-63; https://doi.org/10.3390/gidisord6010004 - 08 Jan 2024
Abstract
►▼
Show Figures
Background: A timely diagnostic colonoscopy (DC) after a positive FIT result is crucial for effective colorectal cancer (CRC) screening. In the Flemish CRC screening program (CRC-SP), 17% of FIT-positive participants had no DC in 2020. This study explores self-reported barriers, experiences, and perceptions
[...] Read more.
Background: A timely diagnostic colonoscopy (DC) after a positive FIT result is crucial for effective colorectal cancer (CRC) screening. In the Flemish CRC screening program (CRC-SP), 17% of FIT-positive participants had no DC in 2020. This study explores self-reported barriers, experiences, and perceptions about DC in FIT-positive participants. Methods: An online survey combining qualitative and quantitative approaches was sent by email to FIT-positive participants (November 2019–September 2020). Results: Out of 5134 invitees, 1597 respondents (31.1%) completed the survey. Among them, 77.5% had undergone/planned a DC, while 22.5% were unwilling to undergo a DC. DC perceptions, expectations, and experiences differed among groups; 57% of the ‘DC-performed’ group reported better-than-expected experiences. A substantial portion of the ‘DC-naïve’ group anticipated pain (42%) and embarrassment (30%), while the actual experience in the ‘DC-performed’ group was much lower (6.4% and 3.2%, respectively). GP advice, support from close contacts, and colonoscopy experiencers trigger DC planning, whereas lack of symptoms, false-positive perception, fears, and embarrassment were identified as barriers to DC. Conclusions: The study reveals barriers/facilitators for a DC in the Flemish CRC-SP. The findings inform targeted interventions for improved DC completion and its impact, including patient navigation and testimonial videos of ‘colonoscopy experiencers’ to address DC misperceptions.
Full article
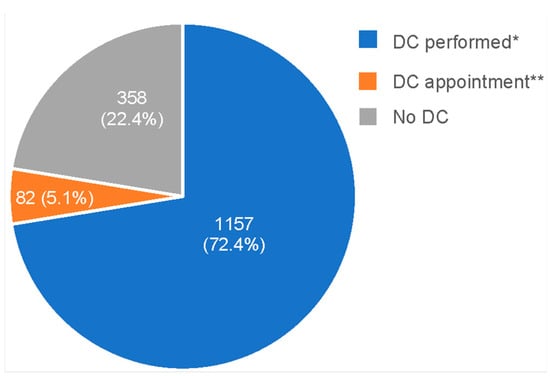
Figure 1
Open AccessArticle
Bleeding and Perforation Complications after Follow-Up Colonoscopies in Faecal Immunochemical Test-Based Colorectal Cancer Screening: Insights from a Retrospective Case–Control Study
by
, , , , , , and
Gastrointest. Disord. 2024, 6(1), 26-48; https://doi.org/10.3390/gidisord6010003 - 05 Jan 2024
Abstract
►▼
Show Figures
Monitoring complications of colonoscopies after a positive faecal immunochemical test (FIT-colonoscopies) is crucial in FIT-based colorectal cancer (CRC) screening. We investigated the occurrence of bleeding and perforation post FIT-colonoscopies (2013–2019) in Flanders and the contributing factors. A retrospective case–control study was conducted, including
[...] Read more.
Monitoring complications of colonoscopies after a positive faecal immunochemical test (FIT-colonoscopies) is crucial in FIT-based colorectal cancer (CRC) screening. We investigated the occurrence of bleeding and perforation post FIT-colonoscopies (2013–2019) in Flanders and the contributing factors. A retrospective case–control study was conducted, including bleeding/perforation cases within 14 days after index colonoscopy, and controls without such events. Bleeding rates dropped from 0.9–1.1% (pre-2017) to 0.3% (2017–2018) and further to 0.05% (2019), while perforation rates remained at 0.05–0.11% (2014–2019). Male gender, polypectomy, general anaesthesia, and recent antiplatelet/antithrombotic drug use increased bleeding odds. Incomplete colonoscopy, polypectomy, general anaesthesia, and recent antiplatelet/antithrombotic drug use raised perforation odds. The endoscopists (n = 16) with highest bleeding rates (top 5%) performed only 6% of total FIT-colonoscopies, yet their patients experienced 45.5% of bleeding events. Similarly, for the top 5% of perforation rates, endoscopists conducting only 4.5% of total FIT-colonoscopy had 49.0% of perforation events occur in their patients. This study sheds light on FIT-colonoscopy-related complications in Flanders, their rates and risk factors. These findings can be incorporated into CRC screening materials and guide interventions to mitigate complications. A central colonoscopy register is currently lacking in Belgium, highlighting the need for its establishment to facilitate recurrent monitoring and evaluation.
Full article
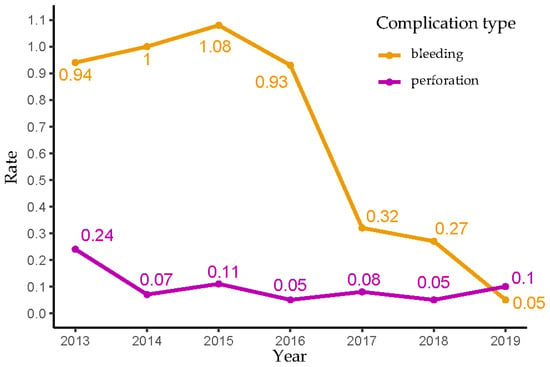
Figure 1
Open AccessArticle
The Treatment Effects of Percutaneous Drainage with or without Sclerotherapy for Symptomatic Liver Cysts
by
, , , , , , , , , , and
Gastrointest. Disord. 2024, 6(1), 13-25; https://doi.org/10.3390/gidisord6010002 - 05 Jan 2024
Abstract
Background: While the current guidelines recommend laparoscopic deroofing for symptomatic simple liver cysts, percutaneous drainage may serve as a less invasive alternative method. In this study, the treatment effects of percutaneous drainage with or without sclerotherapy for symptomatic simple liver cysts were evaluated.
[...] Read more.
Background: While the current guidelines recommend laparoscopic deroofing for symptomatic simple liver cysts, percutaneous drainage may serve as a less invasive alternative method. In this study, the treatment effects of percutaneous drainage with or without sclerotherapy for symptomatic simple liver cysts were evaluated. Methods: Between April 2016 and March 2021, 79 patients who initially required hospitalization due to symptomatic simple liver cysts were enrolled in this multicenter retrospective study. They were treated percutaneously with or without sclerotherapy. The factors associated with symptom recurrence, clinical course and prognosis were investigated. Results: Of the 79 patients treated percutaneously, 11 (13.9%) had symptom recurrence due to liver cysts during the observation period. The maximum diameter of liver cysts at baseline was the only significant factor for the recurrence of these symptoms (p = 0.004). In a receiver operating characteristics analysis, the cut-off of the diameter for symptom recurrence was 16.5 cm. No additional effect of sclerotherapy on drainage was demonstrated in patients with a cyst diameter of <16.5 cm, and in patients with a cyst diameter of ≥16.5 cm, the cumulative recurrence rates of symptoms were significantly lower in the patients treated via sclerotherapy with 5% ethanolamine oleate or with minocycline hydrochloride than in those treated with drainage alone or via sclerotherapy with absolute ethanol. No problematic adverse effects were observed of sclerotherapy. Conclusions: Drainage with sclerotherapy with 5% ethanolamine oleate or minocycline hydrochloride was an effective and safe treatment for patients whose liver cysts had a maximum diameter of ≥16.5 cm. Considering both its efficacy and safety, sclerotherapy with either of these agents is recommended for patients with a maximum liver cyst diameter of ≥16.5 cm.
Full article
(This article belongs to the Topic Advances in Gastrointestinal and Liver Disease: From Physiological Mechanisms to Clinical Practice)
►▼
Show Figures
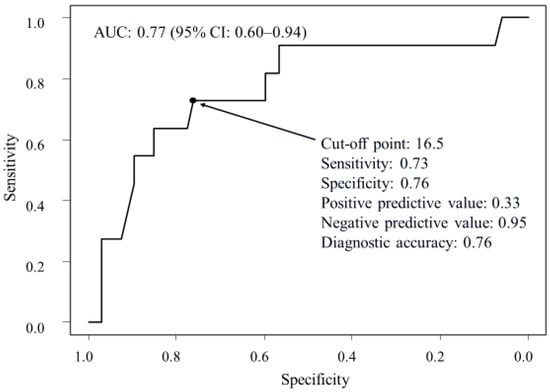
Figure 1
Open AccessArticle
Gastrointestinal Group Education for Children and Adolescents with Functional Abdominal Pain Disorders—A Feasibility Study of a Brief Intervention
by
, , , , and
Gastrointest. Disord. 2024, 6(1), 1-12; https://doi.org/10.3390/gidisord6010001 - 20 Dec 2023
Abstract
Functional abdominal pain disorders are common and disabling in children, but treatment options are limited. In a pilot study, we aimed to investigate if a brief group education program for pediatric patients with functional abdominal pain disorders and their parents is feasible and
[...] Read more.
Functional abdominal pain disorders are common and disabling in children, but treatment options are limited. In a pilot study, we aimed to investigate if a brief group education program for pediatric patients with functional abdominal pain disorders and their parents is feasible and acceptable. Group education in adult irritable bowel syndrome has shown large treatment effects, but it has not been evaluated in children. The gastrointestinal (GI) group education, delivered in the clinic to 23 child–parent dyads, consisted of lectures by a pediatric gastroenterologist, a psychologist, and a dietician. Validated digital questionnaires were filled in by children and parents before and after the intervention. Most participants in the GI group education attended all sessions, and credibility in treatment was deemed high. Children’s self-reported knowledge of functional abdominal pain disorders increased, and improvements in gastrointestinal symptoms were reported at the end of this study. Our findings indicate that group education for children and adolescents with functional abdominal pain disorders, and their parents, is acceptable and feasible and may improve symptoms. A brief group education program may be of benefit in the management of pediatric functional abdominal pain disorders in several cases and when the family needs more knowledge than can be provided in primary care.
Full article
(This article belongs to the Special Issue Pediatric Functional Gastrointestinal Disorders: Challenges in Diagnosis and Treatment)
►▼
Show Figures
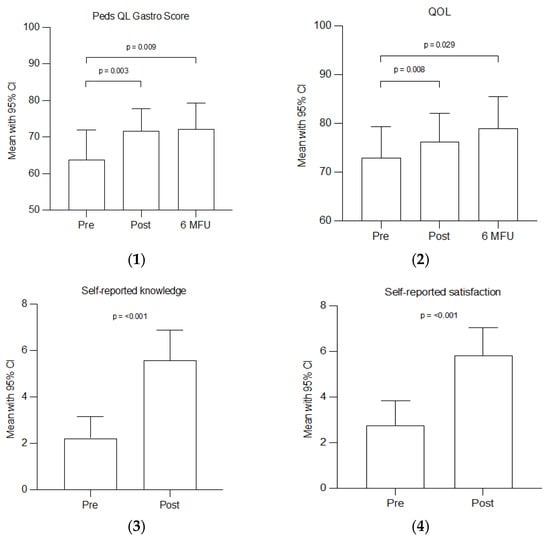
Figure 1
Open AccessReview
Colorectal Cancer Liver Metastasis—State-of-the-Art and Future Perspectives
Gastrointest. Disord. 2023, 5(4), 580-608; https://doi.org/10.3390/gidisord5040046 - 15 Dec 2023
Abstract
The current management of colorectal cancer liver metastasis (CRCLM) patients involves a multidisciplinary approach, with surgical resection remaining the primary curative option. The advances in liver surgery have improved outcomes, enabling more patients to undergo surgery successfully. In addition, the development of imaging
[...] Read more.
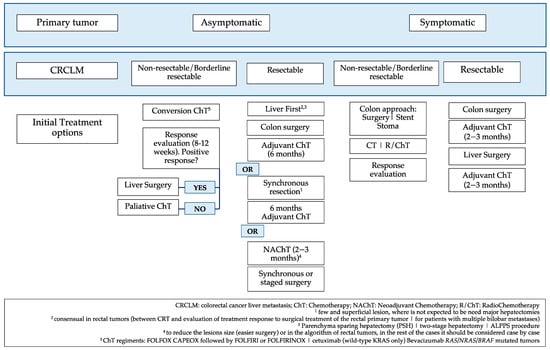
The current management of colorectal cancer liver metastasis (CRCLM) patients involves a multidisciplinary approach, with surgical resection remaining the primary curative option. The advances in liver surgery have improved outcomes, enabling more patients to undergo surgery successfully. In addition, the development of imaging software has improved the preoperative planning and patient selection for surgery and other interventions. Systemic therapies, such as targeted therapies and immunotherapies, have enhanced the chances of complete resection. Targeted agents, in combination with chemotherapy, have shown efficacy in downstaging tumors and increasing resectability. The algorithm approach for these patients continues to evolve, driven by a deeper understanding of the underlying biology. Personalized medicine, guided by molecular profiling and the potential of liquid biopsies in this field, may lead to more tailored treatment strategies. A greater understanding of the immune microenvironment in CRLM may unlock the potential for immune checkpoint inhibitors and novel immunotherapies to become more prominent in the treatment landscape. This review explores the current state-of-the-art treatment of CRCLM and discusses promising future perspectives.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
►▼
Show Figures
Scheme 1
Open AccessSystematic Review
From Algorithms to Clinical Utility: A Systematic Review of Individualized Risk Prediction Models for Colorectal Cancer
by
, , , , , , , and
Gastrointest. Disord. 2023, 5(4), 549-579; https://doi.org/10.3390/gidisord5040045 - 11 Dec 2023
Abstract
►▼
Show Figures
Individualized risk prediction models for colorectal cancer (CRC) play a pivotal role in shaping risk-based screening approaches, garnering attention for use in informed decision making by patients and clinicians. While the incorporation of new predictors and the development of advanced yet complex prediction
[...] Read more.
Individualized risk prediction models for colorectal cancer (CRC) play a pivotal role in shaping risk-based screening approaches, garnering attention for use in informed decision making by patients and clinicians. While the incorporation of new predictors and the development of advanced yet complex prediction models can enhance model performance, their practical implementation in clinical settings remains challenging. This systematic review assessed individualized CRC risk prediction models for their validity and potential clinical utility. Utilizing the Cochrane Collaboration methods and PROBAST tool, we conducted comprehensive searches across key databases and risk of bias assessment, respectively. Out of 41 studies included evaluating 44 risk prediction models, 12 conventional and 3 composite models underwent external validation. All risk models exhibited varying discriminatory accuracy, with the area under the curve (AUCs) ranging from 0.57 to 0.90. However, most studies showed an unclear or high risk of bias, with concerns about applicability. Of the five models with promising clinical utility, only two underwent external validation and one employed a decision curve analysis. These models demonstrated a discriminating and well-calibrated performance. While high-performing CRC risk prediction models exist, a need for transparent reporting of performance metrics and their clinical utility persists. Further research on this area is needed to facilitate the integration of these models into clinical practice, particularly in CRC screening.
Full article
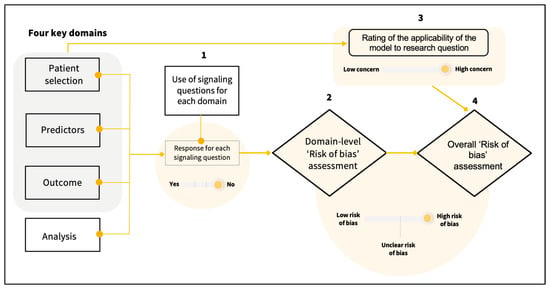
Figure 1
Open AccessArticle
Protection of Testis against Lipopolysaccharide-Induced Toxicity: Mildronate-Induced L-Carnitine Depletion as a Modulator of Gut Microbiome Composition and Gastrointestinal Inflammation
by
, , , , and
Gastrointest. Disord. 2023, 5(4), 536-548; https://doi.org/10.3390/gidisord5040044 - 05 Dec 2023
Abstract
►▼
Show Figures
L-carnitine plays a critical role in sperm functioning and maintaining male fertility. Mildronate is a widely used drug for treating cardiovascular diseases. Mildronate inhibits L-carnitine biosynthesis and transport into cells while increasing glucose supply. Therefore, it is speculated that mildronate may impair male
[...] Read more.
L-carnitine plays a critical role in sperm functioning and maintaining male fertility. Mildronate is a widely used drug for treating cardiovascular diseases. Mildronate inhibits L-carnitine biosynthesis and transport into cells while increasing glucose supply. Therefore, it is speculated that mildronate may impair male fertility by depleting L-carnitine. On the other hand, mildronate is known to have anti-inflammatory effects, which can positively influence the male reproductive system in certain physiological conditions. In this study, we induced inflammation in mice through lipopolysaccharide (LPS) injections and examined some inflammation markers in the testes and intestine, which contribute significantly to the development of systemic inflammation. We demonstrated that mildronate reduces inflammation in mouse testes and preserves mitochondrial DNA integrity. Importantly, mildronate-induced L-carnitine depletion did not have a negative impact on testicular properties or sperm count. We propose that the anti-inflammatory effect of mildronate may be linked to its action on the bacterial composition of the gut microbiome. Mildronate increases the Firmicutes/Bacteroidetes ratio, which is reduced after LPS injections. In contrast to L-carnitine supplementation, mildronate does not decrease the level of Alloprevotella, a bacterial genus that is necessary for reducing inflammation. Additionally, mildronate decreased the expression of pro-inflammatory cytokines and inflammation markers in the intestine, which aligns with our hypothesis regarding its anti-inflammatory effect.
Full article
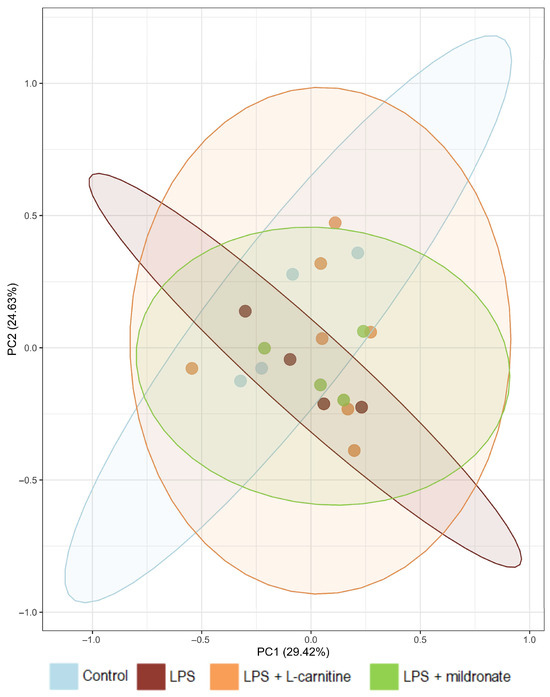
Figure 1
Open AccessReview
Gut–Brain Axis, Microbiota and Probiotics—Current Knowledge on Their Role in Irritable Bowel Syndrome: A Review
by
, , , , , , , , and
Gastrointest. Disord. 2023, 5(4), 517-535; https://doi.org/10.3390/gidisord5040043 - 24 Nov 2023
Abstract
►▼
Show Figures
Irritable bowel syndrome (IBS) is a common digestive disorder with a significant impact on both individuals and society in terms of quality of life and healthcare costs. A growing body of research has identified various communication pathways between the microbiota and the brain
[...] Read more.
Irritable bowel syndrome (IBS) is a common digestive disorder with a significant impact on both individuals and society in terms of quality of life and healthcare costs. A growing body of research has identified various communication pathways between the microbiota and the brain in relation to motility disorders, with the gut–brain axis being key to the pathogenesis of IBS. Multiple factors contribute to the pathogenetic pathways in IBS, including immune mechanisms, psychosocial factors, increased oxidative stress and pro-inflammatory cytokine release, as well as genetic and hormonal factors. Increased permeability of the normal intestinal barrier allows bacterial products to access the lamina propria, providing a mechanism for perpetuating chronic inflammation and characteristic symptoms. The microbiota influences inflammatory processes in IBS by altering the balance between pro-inflammatory factors and host defence. Probiotics modulate the pathophysiological mechanisms involved in IBS by influencing the composition of the microbiota and improving intestinal motility disorders, visceral hypersensitivity, immune function of the intestinal epithelium, metabolic processes in the intestinal lumen, dysfunction of the microbiota-GBA, and are recognised as effective and safe in IBS therapy. Our study aimed to provide a comprehensive overview of the relationship between the gut–brain axis, microbiota, and IBS, based on current information.
Full article
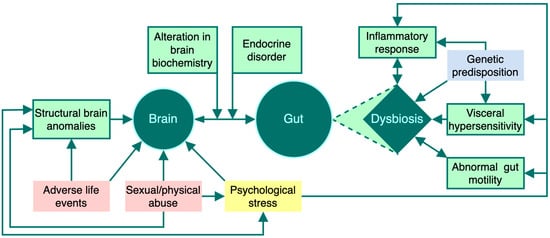
Figure 1
Open AccessArticle
Patient-Reported Outcomes and Survival Following Pancreatic Cancer Resection—Results from a Cross-Section Study
Gastrointest. Disord. 2023, 5(4), 508-516; https://doi.org/10.3390/gidisord5040042 - 21 Nov 2023
Abstract
The aims of this study were to assess patient-reported outcomes and the survival of patients following curative resection for pancreas cancer. Adult patients undergoing curative pancreatic resection between April 2014 and April 2019 across six major hospitals in Sydney were invited to complete
[...] Read more.
The aims of this study were to assess patient-reported outcomes and the survival of patients following curative resection for pancreas cancer. Adult patients undergoing curative pancreatic resection between April 2014 and April 2019 across six major hospitals in Sydney were invited to complete the Short-Form 36 (SF-36v2) and the Functional Assessment Cancer Therapy—Hepatobiliary (FACT-Hep) questionnaires. Time from surgery was categorised into four different time points: 3–11, 12–23, 24–35, and 36–62 months. Survival analyses were performed using Kaplan–Meier and log-rank tests. A total of 278 patients underwent curative resection. Mean (SD) age was 65.0 (13.2), and 50.7% (n = 141) were males. Out of the 205 (74%) alive patients, 128 (62%) completed the study surveys. The physical component score and total FACT-Hep scores showed no significant changes over time. The mental component score improved from 3–11 months to 12–23 months (p = 0.009) and from 3–11 months to 36–62 months (p = 0.007). Survivorship showed a significant difference between malignancy, pre-malignancy, and benign disease groups, with 45.8 months (95%CI: 42.4–49.1), 40.3 months (95%CI: 36.4–44.2), and 41.3 months (95%CI: 37.9–44.9), respectively. For patients undergoing curative resection for pancreatic cancer, mental component scores improved over time, whereas overall survival outcomes seem to be influenced according to cancer pathology.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
►▼
Show Figures
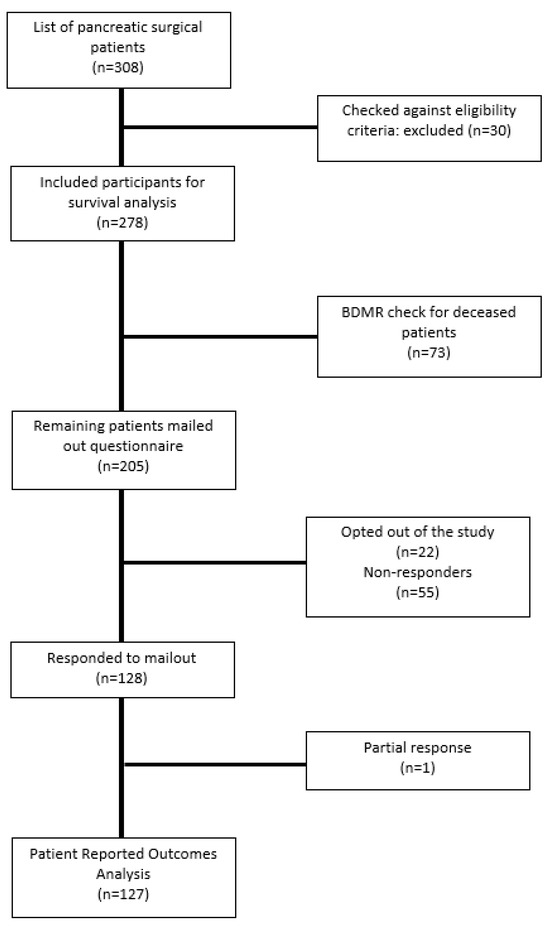
Figure 1
Open AccessReview
An Overview of the Management of Functional Gastrointestinal Disorders in Infancy
by
and
Gastrointest. Disord. 2023, 5(4), 500-507; https://doi.org/10.3390/gidisord5040041 - 15 Nov 2023
Abstract
This review article will address the frequently encountered functional gastrointestinal disorders (FGIDs) occurring in infancy. The clinical features and management of infant regurgitation, infant colic, infant dyschezia, and functional constipation are discussed with reference to the most recent literature and evidence. Management should
[...] Read more.
This review article will address the frequently encountered functional gastrointestinal disorders (FGIDs) occurring in infancy. The clinical features and management of infant regurgitation, infant colic, infant dyschezia, and functional constipation are discussed with reference to the most recent literature and evidence. Management should be focused on ruling out organic causes with careful history and examination, and then reassurance for the caregiver in this often very stressful period of parenting. There is often no or minimal pharmacological treatment necessary for FGIDs and treatment should be individualised for each patient and family.
Full article
(This article belongs to the Special Issue Pediatric Functional Gastrointestinal Disorders: Challenges in Diagnosis and Treatment)
Open AccessArticle
Differentiation between Gastric and Colorectal Adenocarcinomas Based on Maspin, MLH1, PMS2 and K-Ras Concentrations Determined Using Stochastic Sensors
Gastrointest. Disord. 2023, 5(4), 487-499; https://doi.org/10.3390/gidisord5040040 - 06 Nov 2023
Abstract
Background: Gastrointestinal adenocarcinomas are a worldwide and some of the most important causes of death related to cancers. MLH1, PMS2, and K-Ras are some of the main molecules responsible for the control of cellular proliferation. They are widely used as biomarkers for the
[...] Read more.
Background: Gastrointestinal adenocarcinomas are a worldwide and some of the most important causes of death related to cancers. MLH1, PMS2, and K-Ras are some of the main molecules responsible for the control of cellular proliferation. They are widely used as biomarkers for the evaluation of the features of tumoral processes and the clinicopathological characteristics. They depend on the type of cells implied in the tumoral process, and it can be observed in the concentrations of them in different biological fluids. Maspin, also known as peptidase inhibitor 5 or serpin B5 is a tumor suppressor which inhibits invasion and angiogenesis and also regulates apoptosis, but it can also present oncogenic activity depending on tumor location and histology and on the subcellular maspin localization. Its correlations with gastric and colorectal carcinomas have been emphasized in a series of articles, and in this work, a method is used to quantify the concentrations of maspin in three biological fluids, allowing correlations with pathological features. Methods: Patients with their clinical and pathological features were selected from the database of the project GRAPHSENSGASTROINTES and used accordingly with the Ethics committee approval nr. 32647/2018 awarded by the County Emergency Hospital from Targu-Mures. Three kinds of samples have been analyzed (saliva, whole blood, and urine) using a stochastic method using stochastic microsensors. Results: The results obtained using stochastic sensors were correlated with the location of cancer, and there have been elaborated a series of criteria to differentiate gastric cancers from colorectal ones. Conclusions: There can be differentiation between the two types of cancers by using the concentrations of MLH1, PMS2, and K-Ras in saliva and urine samples or the levels of maspin in whole blood and urine or in whole blood, urine, and saliva. The data analysis led to a series of criteria for evaluation of the cancer location. Using only MLH1 and PMS2 concentrations in one of the two kinds of samples was only indicative and did not cover most cases. The use of the criteria only for MLH1 and PMS2 increased the probability of finding out the location, but the best results require the concentrations of K-Ras in the two kinds of samples as additional criteria.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
►▼
Show Figures
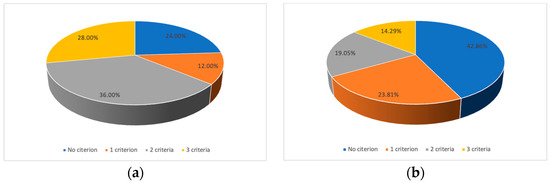
Figure 1
Open AccessArticle
Excessive Glucose and Fructose Intake Aggravates the Pathogenesis of Rat Experimental Colitis
by
, , , , , , , and
Gastrointest. Disord. 2023, 5(4), 474-486; https://doi.org/10.3390/gidisord5040039 - 06 Nov 2023
Abstract
►▼
Show Figures
Ulcerative colitis (UC) is a relapsing and remitting disease that causes chronic inflammation and ulceration of colonic tissue, especially in the rectum region. Although sugars are rapidly digested and absorbed and can be efficiently utilized as energy in the body, they are also
[...] Read more.
Ulcerative colitis (UC) is a relapsing and remitting disease that causes chronic inflammation and ulceration of colonic tissue, especially in the rectum region. Although sugars are rapidly digested and absorbed and can be efficiently utilized as energy in the body, they are also known to promote inflammation. Herein, we aimed to examine the effects of special diets containing excess glucose (Glu) or fructose (Fru) on the pathogenesis of dextran sulfate sodium (DSS)-induced UC in Wistar rats. The model rats (termed UC rats or UCR) were divided into three groups: DSS group, UCR fed a regular diet; DSS + Glu group, UCR fed a special diet mixed with glucose at 63% calories; DSS + Fru group, UCR fed a special diet mixed with fructose at 63% calories. The DSS + Glu and DSS + Fru groups exhibited a lower weight and colon length than the DSS group. The DSS + Fru group had a lower diet and DSS intake than the other two groups. The microscopic findings revealed that the DSS + Glu and DSS + Fru groups tended to have higher severity scores than the DSS group. The DSS + Fru group tended to have higher serum and colonic tissue concentrations of inflammatory cytokines than the DSS + Glu group. Collectively, these findings suggest that excessive glucose and fructose intake can aggravate intestinal inflammation.
Full article
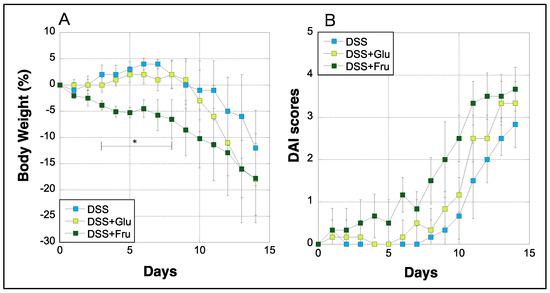
Figure 1
Open AccessArticle
Low Short-Chain-Fatty-Acid-Producing Activity of the Gut Microbiota Is Associated with Hypercholesterolemia and Liver Fibrosis in Patients with Metabolic-Associated (Non-Alcoholic) Fatty Liver Disease
by
, , , , , , and
Gastrointest. Disord. 2023, 5(4), 464-473; https://doi.org/10.3390/gidisord5040038 - 30 Oct 2023
Abstract
The aim of this study was to investigate the short-chain fatty acid (SCFA) activity of the gut microbiota of patients with metabolic-associated fatty liver disease (MAFLD). The level and spectrum of short-chain fatty acids (SCFAs) were determined via gas–liquid chromatography. Liver fibrosis was
[...] Read more.
The aim of this study was to investigate the short-chain fatty acid (SCFA) activity of the gut microbiota of patients with metabolic-associated fatty liver disease (MAFLD). The level and spectrum of short-chain fatty acids (SCFAs) were determined via gas–liquid chromatography. Liver fibrosis was assessed using the FIB-4 index and elastography. Among 42 non-cirrhotic MAFLD patients, 24 had high fecal SCFA levels (group H) and 18 had low fecal SCFA levels (group L). Patients in group H had lower serum uric acid, total cholesterol, and LDL cholesterol levels but a higher BMI than those in group L. All patients in group L and only 37.9% of those in group H were found to have hypercholesterolemia. In patients with hypercholesterolemia, the level of SCFAs was lower than that in patients without hypercholesterolemia. Patients in group H had less liver fibrosis than patients in group L. A total of 50.0% of the patients in group H and 92.3% of those in group L had significant liver fibrosis (≥F2). Patients with significant liver fibrosis had lower levels of fecal SCFAs—particularly acetate and butyrate. The fecal SCFA levels were positively correlated with gamma-glutamyl transferase, total bilirubin levels, BMI, and platelet count and were negatively correlated with FIB-4, liver stiffness, serum total, and LDL cholesterol levels.
Full article
(This article belongs to the Topic Gut Microbiota in Human Health)
►▼
Show Figures
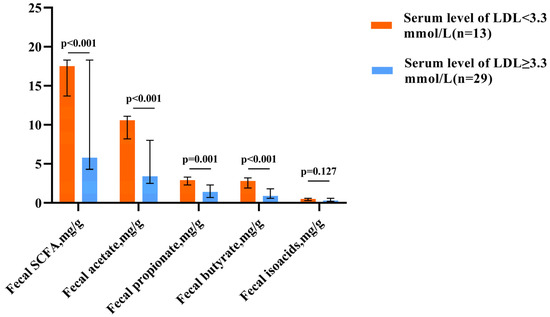
Figure 1
Open AccessArticle
Incidence, Clinicopathological Features and Oncologic Outcome of Appendiceal Neoplasms: A Single-Center Cohort Study
by
, , , , , , and
Gastrointest. Disord. 2023, 5(4), 455-463; https://doi.org/10.3390/gidisord5040037 - 17 Oct 2023
Abstract
►▼
Show Figures
Appendiceal tumors represent a large amalgam of different tumor lineages. The continuous evolution in their pathological classifications has led to some variable recommended attitudes over time. The aim of this study is to review the incidence, clinicopathological characteristics, therapeutic approach and oncological results
[...] Read more.
Appendiceal tumors represent a large amalgam of different tumor lineages. The continuous evolution in their pathological classifications has led to some variable recommended attitudes over time. The aim of this study is to review the incidence, clinicopathological characteristics, therapeutic approach and oncological results in this type of tumor at our institution. This is a single-centre retrospective cohort study. Every pathologic report catalogued as an appendiceal specimen was reviewed for a time period of 5 years (2013–2017) at our institution. Demographic, clinical, pathological and oncologic follow-up data were recorded. A descriptive study of the sample was completed. A total of 1434 appendiceal specimens was analyzed. Appendiceal neoplasms incidence was 3.2%. Epithelial tumors were the predominant histological subtype, making up 68% of the cases. Low-grade appendiceal mucinous neoplasia and neuroendocrine tumors were the most frequent neoplasms with malignant potential, with 13 and 6 cases, respectively. In more than 80% of neoplasia cases, the definitive treatment was appendectomy. Mortality cases were related to tumors with a very poor prognosis and an advanced stage. All patients had adequate oncological follow-up. Although it is still quite rare, the incidence of appendiceal tumors is increasing with an epidemiological change in favor of mucinous neoplasms currently predominating. Therefore, it is necessary to know and use an updated anatomo-pathological classification in order to provide correct treatment in the first or second surgical stage, as well as the correct follow-up of patients.
Full article
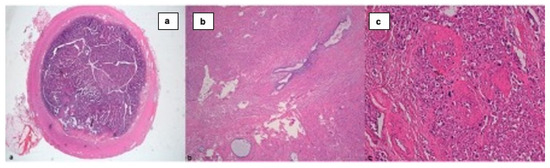
Figure 1
Open AccessArticle
Scientific and Public Interest in Bariatric Surgery for Obesity: The Italian Scenario
by
, , , , , , and
Gastrointest. Disord. 2023, 5(4), 438-454; https://doi.org/10.3390/gidisord5040036 - 11 Oct 2023
Cited by 2
Abstract
►▼
Show Figures
Background: Obesity is an escalating concern in our society. Bariatric surgery appears to be the only feasible alternative for severe obesity. This study aims to conduct an integrative analysis of the Italian context concerning bariatric surgery, with a specific focus on the surgical
[...] Read more.
Background: Obesity is an escalating concern in our society. Bariatric surgery appears to be the only feasible alternative for severe obesity. This study aims to conduct an integrative analysis of the Italian context concerning bariatric surgery, with a specific focus on the surgical procedures of sleeve gastrectomy, mini-gastric bypass, and gastric bypass. Methods: The analysis is based on bibliometric data extracted from the Scopus database to find Italian publications in this field from 2012 to 2022. Along with scientific interest, it is essential to assess the level of public interest in these topics. Google Trends is the most extensively utilized free tool for the analysis of online behavior. Using Google Trends data, we analyzed the amount of internet volume searches (Relative Search Volume = RSV) for the Italian terms “sleeve gastrectomy”, “mini-gastric bypass” and “gastric bypass”, both temporally (from 2012 to 2022 years) and geographically. Furthermore, to illustrate the Italian landscape, we compared Google Trends data with data from the Italian registry “Società Italiana di Chirurgia dell’Obesità e delle malattie metaboliche” (SICOB), which includes information about bariatric surgery procedures performed in the country. Results: Over the past decade, there has been a significant increase in the scientific literature on sleeve gastrectomy, mini-gastric bypass, and gastric bypass surgeries in Italy. Google Trends data has shown an increase in online public interest in these surgical procedures, from 2012 to 2022. The examination of the Google Trends information combined with the SICOB data demonstrated a remarkable association between the two data sets. Conclusions: Bariatric surgery has increased quickly in Italy in terms of scientific research and surgical interventions. The analysis of Google Trends data in conjunction with data from SICOB has revealed an interesting correlation between the two datasets therefore, Google Trends can be useful for estimating the demand for bariatric surgical procedures.
Full article
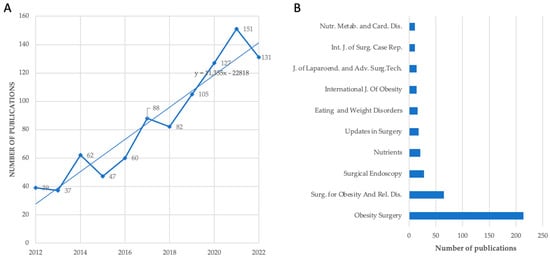
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomedicines, Current Oncology, Diagnostics, Gastrointestinal Disorders, JCM
Advances in Gastrointestinal and Liver Disease: From Physiological Mechanisms to Clinical Practice
Topic Editors: Davide Giuseppe Ribaldone, Gian Paolo CavigliaDeadline: 20 June 2024
Topic in
Cancers, Diagnostics, JCM, Current Oncology, Gastrointestinal Disorders, Biomedicines
Hepatobiliary and Pancreatic Diseases: Novel Strategies of Diagnosis and Treatments
Topic Editors: Alessandro Coppola, Damiano Caputo, Roberta Angelico, Domenech Asbun, Chiara MazzarelliDeadline: 20 July 2024

Conferences
Special Issues
Special Issue in
Gastrointestinal Disorders
Factors Affecting Disease Activity in Children and Adults with Inflammatory Bowel Disease: An Exploration of Pro-Inflammatory and Anti-Inflammatory Elements
Guest Editors: Angharad Hurley (Vernon-Roberts), Andrew DayDeadline: 30 September 2024
Special Issue in
Gastrointestinal Disorders
Feature Papers in Gastrointestinal Disorders in 2023-2024
Guest Editor: Richard W. McCallumDeadline: 31 December 2024






.jpg)





