Journal Description
Neurology International
Neurology International
is an international, peer-reviewed, open access journal which provides an advanced forum for studies related to all aspects of neurology and neuroscience, published bimonthly online by MDPI (from Volume 12 issue 3 - 2020).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 23.3 days after submission; acceptance to publication is undertaken in 3.9 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
3.0 (2022);
5-Year Impact Factor:
2.2 (2022)
Latest Articles
Extra-Axial Cavernous Angioma: A Case Report and Review of the Literature
Neurol. Int. 2024, 16(1), 162-185; https://doi.org/10.3390/neurolint16010010 - 12 Jan 2024
Abstract
►
Show Figures
Cavernous angiomas (CAs) are benign vascular malformations predominantly seen in the brain parenchyma and therefore referred to as intra-axial. Extra-axial dural-based cavernous angiomas, on the other hand, are rare vascular lesions found outside of the brain parenchyma. They occur in the middle fossa
[...] Read more.
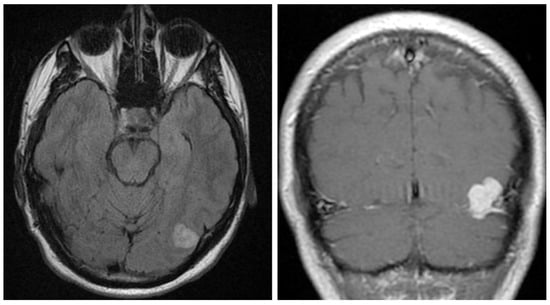
Cavernous angiomas (CAs) are benign vascular malformations predominantly seen in the brain parenchyma and therefore referred to as intra-axial. Extra-axial dural-based cavernous angiomas, on the other hand, are rare vascular lesions found outside of the brain parenchyma. They occur in the middle fossa and may be easily misdiagnosed as meningiomas due to their extra-axial location. In addition, CAs that are located outside the middle fossa, such as in the convexity, have a better prognosis since they are more surgically accessible. Surgical resection is the main treatment of choice in CAs. However, other options, such as embolization and radiotherapy, may also be considered therapeutic choices or additive treatment options. The pathogenesis of CA and the involvement of other factors (genetics or environmental factors) are still unknown and require further investigation. We are presenting a young man who presented for evaluation of seizure-like events without any family history of neurologic conditions. The physical examination was unremarkable except for a slightly antalgic gait. Imaging studies showed an extra-axial left tentorial mass suggestive of a meningioma, hemangiopericytoma, or other extra-axial lesions. The lesion was resected where its vascular nature was mentioned initially, and the histology proved the diagnosis of cavernous angioma. Here we give an overview of the known pathogenesis, causes, clinical features, and diagnostic and therapeutic options in CA. Better knowledge about CA, its causes, clinical features, and treatment options would help clinicians in early diagnosis and patient management.
Full article
Open AccessSystematic Review
Pulmonary Function Tests Post-Stroke. Correlation between Lung Function, Severity of Stroke, and Improvement after Respiratory Muscle Training
by
, , , , , , , , , , , and
Neurol. Int. 2024, 16(1), 139-161; https://doi.org/10.3390/neurolint16010009 - 11 Jan 2024
Abstract
Stroke is a significant cause of mortality and chronic morbidity caused by cardiovascular disease. Respiratory muscles can be affected in stroke survivors, leading to stroke complications, such as respiratory infections. Respiratory function can be assessed using pulmonary function tests (PFTs). Data regarding PFTs
[...] Read more.
Stroke is a significant cause of mortality and chronic morbidity caused by cardiovascular disease. Respiratory muscles can be affected in stroke survivors, leading to stroke complications, such as respiratory infections. Respiratory function can be assessed using pulmonary function tests (PFTs). Data regarding PFTs in stroke survivors are limited. We reviewed the correlation between PFTs and stroke severity or degree of disability. Furthermore, we reviewed the PFT change in stroke patients undergoing a respiratory muscle training program. We searched PubMed until September 2023 using inclusion and exclusion criteria in order to identify studies reporting PFTs post-stroke and their change after a respiratory muscle training program. Outcomes included lung function parameters (FEV1, FVC, PEF, MIP and MEP) were measured in acute or chronic stroke survivors. We identified 22 studies of stroke patients, who had undergone PFTs and 24 randomised controlled trials in stroke patients having PFTs after respiratory muscle training. The number of patients included was limited and studies were characterised by great heterogeneity regarding the studied population and the applied intervention. In general, PFTs were significantly reduced compared to healthy controls and predicted normal values and associated with stroke severity. Furthermore, we found that respiratory muscle training was associated with significant improvement in various PFT parameters and functional stroke parameters. PFTs are associated with stroke severity and are improved after respiratory muscle training.
Full article
(This article belongs to the Special Issue Treatment Strategy and Mechanism of Acute Ischemic Stroke)
►▼
Show Figures
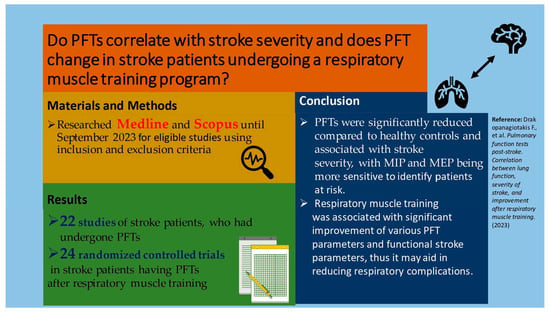
Graphical abstract
Open AccessArticle
Contingent Negative Variation in the Evaluation of Neurocognitive Disorders Due to Possible Alzheimer’s Disease
by
, , , , , and
Neurol. Int. 2024, 16(1), 126-138; https://doi.org/10.3390/neurolint16010008 - 11 Jan 2024
Abstract
The usefulness of Contingent Negative Variation (CNV) potential as a biomarker of neurocognitive disorders due to possible Alzheimer’s disease, is based on its possible physiological correlates. However, its application in the diagnostic evaluation of these disorders is still incipient. The aim of this
[...] Read more.
The usefulness of Contingent Negative Variation (CNV) potential as a biomarker of neurocognitive disorders due to possible Alzheimer’s disease, is based on its possible physiological correlates. However, its application in the diagnostic evaluation of these disorders is still incipient. The aim of this study is to characterize the patterns of cognitive processing of information in the domain of nonspecific global attention, by recording potential CNV in a group of patients with neurocognitive disorders due to possible Alzheimer’s disease. An experimental study of cases and controls was carried out. The sample included 39 patients classified according to DSM-5 with a neurocognitive disorder subtype possibly due Alzheimer’s disease, and a Control Group of 53 subjects with normal cognitive functions. CNV potential was registered using standard protocol. The analysis of variance obtained significant differences in mean values and confidence intervals of total CNV amplitude between the three study groups. The late CNV segment amplitudes makes it possible to discriminate between the level of mild and major dysfunction in the group of patients. The CNV total amplitudes of potential allows for effective discrimination between normal cognitive functioning and neurocognitive disorders due to possible Alzheimer’s disease.
Full article
(This article belongs to the Topic Translational Advances in Neurodegenerative Dementias)
►▼
Show Figures
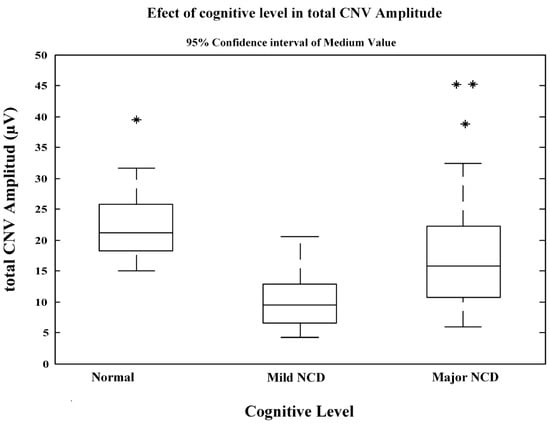
Figure 1
Open AccessArticle
Variability of the Cervical Branch Depending on the Facial Nerve Branching Pattern and Anthropometric Type of the Head
by
, , , , , , and
Neurol. Int. 2024, 16(1), 113-125; https://doi.org/10.3390/neurolint16010007 - 04 Jan 2024
Abstract
►▼
Show Figures
(1) Background: Considering that the specialty literature supplies only general data about the variability of the cervical branch of the facial nerve, this study aimed to determine this branch’s variation and individual peculiarities depending on the nerve branching pattern and anthropometric type of
[...] Read more.
(1) Background: Considering that the specialty literature supplies only general data about the variability of the cervical branch of the facial nerve, this study aimed to determine this branch’s variation and individual peculiarities depending on the nerve branching pattern and anthropometric type of the head. (2) Methods: The study was conducted on 75 hemifaces of adult formalized cadavers. Ahead of anatomical dissection, each head was measured to establish the anthropometric type, according to Franco and colleagues. The branching patterns were then distributed according to the Davis classification. (3) Results: The number of cervical branches (CB) of the facial nerve varied from one to five branches, with the following rate: 1 CB (61.3%), 2 CB (28%), 3 CB (6.7%), 4 CB (2.7%), and 5 CB (1.3%). Seven branching patterns of the facial nerve were revealed: Type I in 18.7%, Type II in 14.7%, Type III in 20%, Type IV in 14.6%, Type V in 5.3%, Type VI in 18.7%, and Type NI in 8% (bizarre types). According to the branching pattern, the mean numbers of the cervical branches were as follows: Type I—1.6 ± 1.02; Type II—1.4 ± 0.50; Type III—1.4 ± 0.50; Type IV—1.4 ± 0.67; Type V—2.0 ± 1.41; Type VI—1.8 ± 1.12; and Type-NI—1.8 ± 0.75; p = 0.599. According to the anthropometric type of the head, the mean number of CB in the mesocephalic type (MCT) was 1.5 ± 0.82, in the dolichocephalic type (DCT), 1.7 ± 0.87, and in the brachycephalic type, (BCT) 1.8 ± 1.04; p = 0.668. (4) Conclusions: The cervical branch of the facial nerve varies depending on the facial nerve branching pattern and the anthropometric type of the head. The highest degree of variation was characteristic of BCT and Type V and the lowest, of MCT and Types II, III, and IV.
Full article
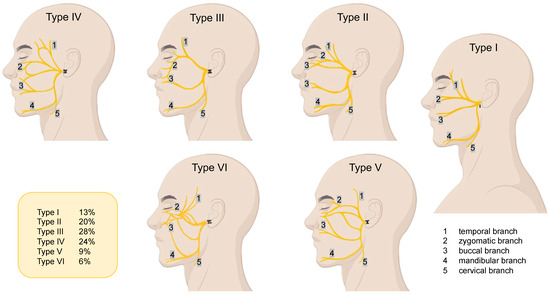
Figure 1
Open AccessReview
Post-Traumatic Cerebral Infarction: A Narrative Review of Pathophysiology, Diagnosis, and Treatment
by
, , , , , , , , and
Neurol. Int. 2024, 16(1), 95-112; https://doi.org/10.3390/neurolint16010006 - 04 Jan 2024
Abstract
►▼
Show Figures
Traumatic brain injury (TBI) is a common diagnosis requiring acute hospitalization. Long-term, TBI is a significant source of health and socioeconomic impact in the United States and globally. The goal of clinicians who manage TBI is to prevent secondary brain injury. In this
[...] Read more.
Traumatic brain injury (TBI) is a common diagnosis requiring acute hospitalization. Long-term, TBI is a significant source of health and socioeconomic impact in the United States and globally. The goal of clinicians who manage TBI is to prevent secondary brain injury. In this population, post-traumatic cerebral infarction (PTCI) acutely after TBI is an important but under-recognized complication that is associated with negative functional outcomes. In this comprehensive review, we describe the incidence and pathophysiology of PTCI. We then discuss the diagnostic and treatment approaches for the most common etiologies of isolated PTCI, including brain herniation syndromes, cervical artery dissection, venous thrombosis, and post-traumatic vasospasm. In addition to these mechanisms, hypercoagulability and microcirculatory failure can also exacerbate ischemia. We aim to highlight the importance of this condition and future clinical research needs with the goal of improving patient outcomes after TBI.
Full article
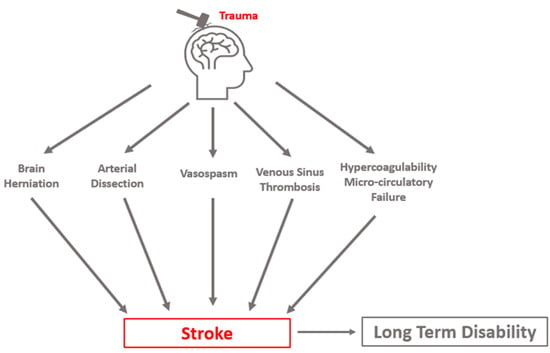
Figure 1
Open AccessReview
The Management of Intracranial Aneurysms: Current Trends and Future Directions
by
, , , , , and
Neurol. Int. 2024, 16(1), 74-94; https://doi.org/10.3390/neurolint16010005 - 03 Jan 2024
Abstract
Intracranial aneurysms represent a major global health burden. Rupture of an intracranial aneurysm is a catastrophic event. Without access to treatment, the fatality rate is 50% in the first 30 days. Over the last three decades, treatment approaches for intracranial aneurysms have changed
[...] Read more.
Intracranial aneurysms represent a major global health burden. Rupture of an intracranial aneurysm is a catastrophic event. Without access to treatment, the fatality rate is 50% in the first 30 days. Over the last three decades, treatment approaches for intracranial aneurysms have changed dramatically. There have been improvements in the medical management of aneurysmal subarachnoid haemorrhage, and there has been an evolution of treatment strategies. Endovascular therapy is now the mainstay of the treatment of ruptured intracranial aneurysms based on robust randomised controlled trial data. There is now an expansion of treatment indications for unruptured intracranial aneurysms to prevent rupture with both microsurgical clipping and endovascular treatment. Both microsurgical and endovascular treatment modalities have evolved, in particular with the introduction of innovative endovascular treatment options including flow diversion and intra-saccular flow disruption. These novel therapies allow clinicians to treat more complex and previously untreatable aneurysms. We aim to review the evolution of treatment strategies for intracranial aneurysms over time, and discuss emerging technologies that could further improve treatment safety and functional outcomes for patients with an intracranial aneurysm.
Full article
(This article belongs to the Special Issue Global Burden of Neurological Disorder)
►▼
Show Figures
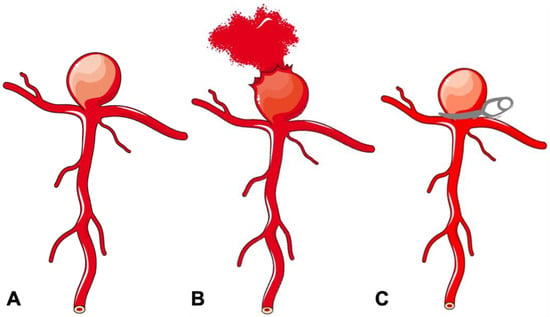
Figure 1
Open AccessArticle
Longitudinal Neuropsychological Assessment of Symptomatic Edema after Subthalamic Nucleus Deep Brain Stimulation Surgery: A Case Series Study
by
, , , , , , , , , , , , , , and
Neurol. Int. 2024, 16(1), 62-73; https://doi.org/10.3390/neurolint16010004 - 28 Dec 2023
Abstract
►▼
Show Figures
Severe non-infectious or non-haemorrhagic brain edema surrounding the electrode represents a rare complication of subthalamic nucleus deep brain stimulation (STN-DBS) surgery. The aim of this study is to report three patients with advanced Parkinson’s Disease (PD) who developed symptomatic brain edema after STN-DBS
[...] Read more.
Severe non-infectious or non-haemorrhagic brain edema surrounding the electrode represents a rare complication of subthalamic nucleus deep brain stimulation (STN-DBS) surgery. The aim of this study is to report three patients with advanced Parkinson’s Disease (PD) who developed symptomatic brain edema after STN-DBS surgery treated with intravenous steroids with a specific profile of reversible cognitive alterations. Patients were both assessed with a comprehensive neuropsychological battery including attention, memory, visuo-spatial and executive tasks. They were also briefly assessed for emotional and behavioural alterations, and for possible limitations in the activities of daily living. Normative data for an Italian population were available for all neuropsychological tests. The patients were firstly assessed before the surgery (baseline) as soon as they became symptomatic for the post-surgery edema and a few more times in follow-up up to ten months. In all patients we observed the resolution of cognitive deficits within six months after surgery with the corresponding reabsorption of edema at brain CT scans. The appearance of post-DBS edema is a fairly frequent and clinically benign event. However, in some rare cases it can be very marked and lead to important clinical—albeit transient—disturbances. These events can compromise, at least from a psychological point of view, the delicate path of patients who undergo DBS and can prolong the post-operative hospital stay. In this setting it could be helpful to perform a brain CT scan in 2–3 days with the aim of detecting the early appearance of edema and treating it before it can constitute a relevant clinical problem.
Full article
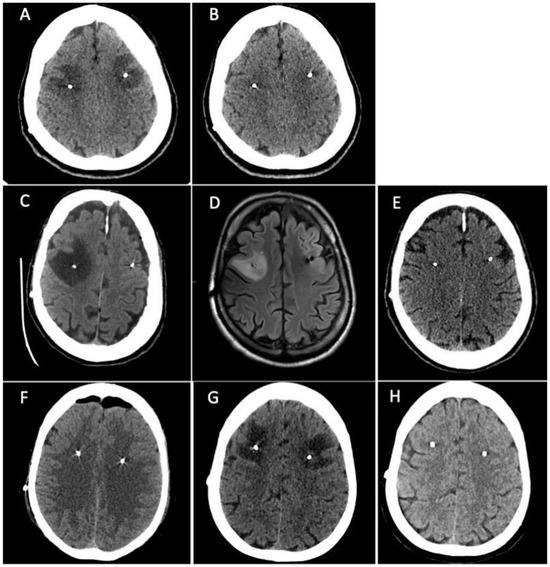
Figure 1
Open AccessArticle
Investigating the Protective Effects of a Citrus Flavonoid on the Retardation Morphogenesis of the Oligodendroglia-like Cell Line by Rnd2 Knockdown
by
, , , , , , , and
Neurol. Int. 2024, 16(1), 33-61; https://doi.org/10.3390/neurolint16010003 - 26 Dec 2023
Abstract
Recent discoveries suggest links between abnormalities in cell morphogenesis in the brain and the functional deficiency of molecules controlling signal transduction in glial cells such as oligodendroglia. Rnd2 is one such molecule and one of the Rho family monomeric GTP-binding proteins. Despite the
[...] Read more.
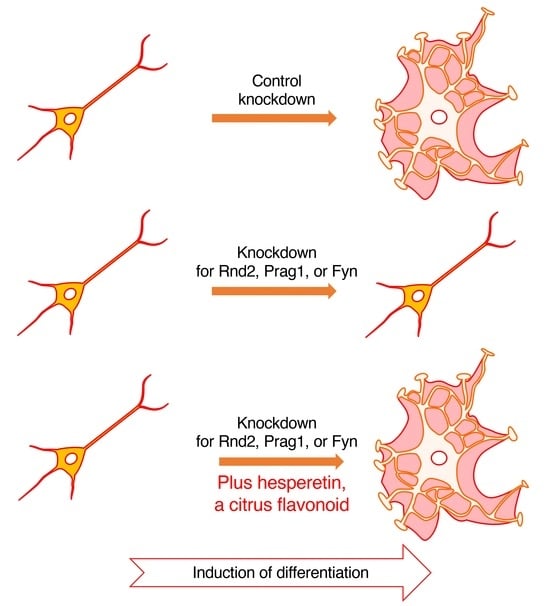
Recent discoveries suggest links between abnormalities in cell morphogenesis in the brain and the functional deficiency of molecules controlling signal transduction in glial cells such as oligodendroglia. Rnd2 is one such molecule and one of the Rho family monomeric GTP-binding proteins. Despite the currently known functions of Rnd2, its precise roles as it relates to cell morphogenesis and disease state remain to be elucidated. First, we showed that signaling through the loss of function of the rnd2 gene affected the regulation of oligodendroglial cell-like morphological differentiation using the FBD-102b cell line, which is often utilized as a differentiation model. The knockdown of Rnd2 using the clustered regularly interspaced palindromic repeats (CRISPR)/CasRx system or RNA interference was shown to slow morphological differentiation. Second, the knockdown of Prag1 or Fyn kinase, a signaling molecule acting downstream of Rnd2, slowed differentiation. Rnd2 or Prag1 knockdown also decreased Fyn phosphorylation, which is critical for its activation and for oligodendroglial cell differentiation and myelination. Of note, hesperetin, a citrus flavonoid with protective effects on oligodendroglial cells and neurons, can recover differentiation states induced by the knockdown of Rnd2/Prag1/Fyn. Here, we showed that signaling through Rnd2/Prag1/Fyn is involved in the regulation of oligodendroglial cell-like morphological differentiation. The effects of knocking down the signaling cascade molecule can be recovered by hesperetin, highlighting an important molecular structure involved in morphological differentiation.
Full article
(This article belongs to the Special Issue Selected Papers from "Brainstorming Research Assembly for Young Neuroscientists (BraYn))
►▼
Show Figures
Graphical abstract
Open AccessSystematic Review
Phantosmia in Parkinson’s Disease: A Systematic Review of the Phenomenology of Olfactory Hallucinations
by
, , , , , , , , and
Neurol. Int. 2024, 16(1), 20-32; https://doi.org/10.3390/neurolint16010002 - 22 Dec 2023
Abstract
►▼
Show Figures
Olfactory dysfunction is a prevalent non-motor symptom in Parkinson’s disease (PD), affecting approximately 65–90% of subjects. PD patients may also report odor perception in the absence of any external source, often referred to as olfactory hallucinations (OHs) or phantosmia. This study aims to
[...] Read more.
Olfactory dysfunction is a prevalent non-motor symptom in Parkinson’s disease (PD), affecting approximately 65–90% of subjects. PD patients may also report odor perception in the absence of any external source, often referred to as olfactory hallucinations (OHs) or phantosmia. This study aims to explore the current understanding of OHs in PD and offer a comprehensive overview of their prevalence and characteristics. We conducted a systematic search of the literature published on PubMed from inception to July 2023 regarding OHs in PD, following PRISMA guidelines. From the 2875 studies identified through database searching, 29 studies fulfilled the necessary criteria and underwent data extraction. The frequency of OHs in PD patients varies widely, ranging from 0.5% to 18.2%, with female prevalence ranging from 36% to 75% of the patients. Olfactory experiences may vary widely, ranging from pleasant scents to unpleasant odors. Several studies have indicated the concurrent presence of other types of hallucinations alongside phantosmia, especially visual and auditory hallucinations. OHs in PD are a type of hallucination that has been largely overlooked. To gain a deeper understanding of OHs in PD patients, the next crucial step should involve the development and validation of a dedicated questionnaire.
Full article
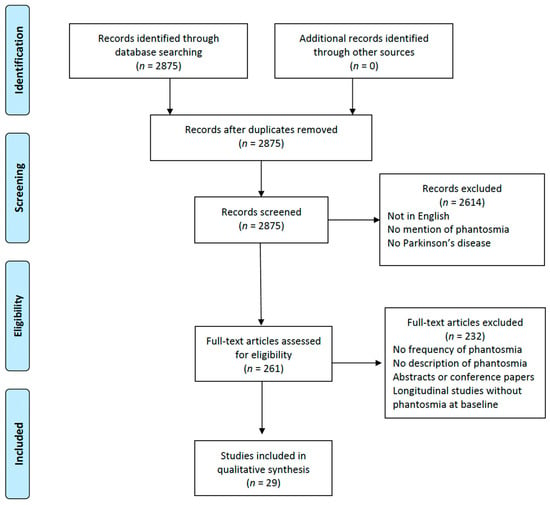
Figure 1
Open AccessSystematic Review
Planimetric and Volumetric Brainstem MRI Markers in Progressive Supranuclear Palsy, Multiple System Atrophy, and Corticobasal Syndrome. A Systematic Review and Meta-Analysis
Neurol. Int. 2024, 16(1), 1-19; https://doi.org/10.3390/neurolint16010001 - 19 Dec 2023
Abstract
►▼
Show Figures
Background: Various MRI markers—including midbrain and pons areas (Marea, Parea) and volumes (Mvol, Pvol), ratios (M/Parea, M/Pvol), and composite markers (magnetic resonance imaging Parkinsonism Indices 1,2; MRPI 1,2)—have been proposed as
[...] Read more.
Background: Various MRI markers—including midbrain and pons areas (Marea, Parea) and volumes (Mvol, Pvol), ratios (M/Parea, M/Pvol), and composite markers (magnetic resonance imaging Parkinsonism Indices 1,2; MRPI 1,2)—have been proposed as imaging markers of Richardson’s syndrome (RS) and multiple system atrophy–Parkinsonism (MSA-P). A systematic review/meta-analysis of relevant studies aiming to compare the diagnostic accuracy of these imaging markers is lacking. Methods: Pubmed and Scopus were searched for studies with >10 patients (RS, MSA-P or CBS) and >10 controls with data on Marea, Parea, Mvol, Pvol, M/Parea, M/Pvol, MRPI 1, and MRPI 2. Cohen’s d, as a measure of effect size, was calculated for all markers in RS, MSA-P, and CBS. Results: Twenty-five studies on RS, five studies on MSA-P, and four studies on CBS were included. Midbrain area provided the greatest effect size for differentiating RS from controls (Cohen’s d = −3.10; p < 0.001), followed by M/Parea and MRPI 1. MSA-P had decreased midbrain and pontine areas. Included studies exhibited high heterogeneity, whereas publication bias was low. Conclusions: Midbrain area is the optimal MRI marker for RS, and pons area is optimal for MSA-P. M/Parea and MRPIs produce smaller effect sizes for differentiating RS from controls.
Full article
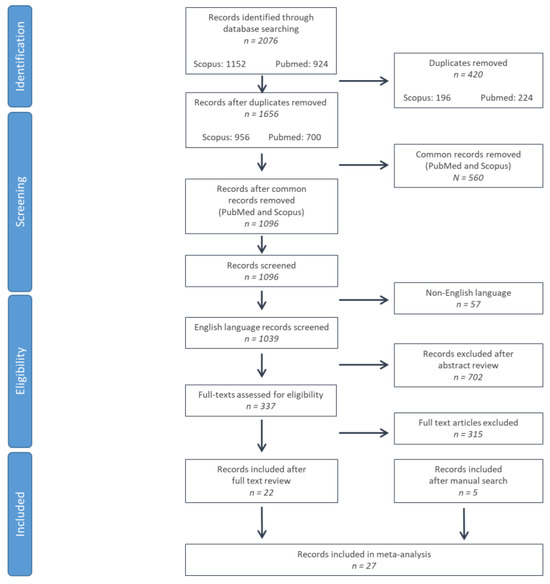
Figure 1
Open AccessCase Report
The Beneficial Outcome of Subsequent Treatment with Anakinra during the Chronic Phase of Febrile Infection-Related Epilepsy Syndrome (FIRES): A Case Report
Neurol. Int. 2023, 15(4), 1489-1496; https://doi.org/10.3390/neurolint15040097 - 11 Dec 2023
Abstract
►▼
Show Figures
This case report presents the clinical course of an eight-year-old boy diagnosed with febrile infection-related epilepsy syndrome (FIRES) at the age of four. Following a febrile infection, the patient experienced his initial episode of serial generalized clonic seizures. The severity of his condition
[...] Read more.
This case report presents the clinical course of an eight-year-old boy diagnosed with febrile infection-related epilepsy syndrome (FIRES) at the age of four. Following a febrile infection, the patient experienced his initial episode of serial generalized clonic seizures. The severity of his condition led to 11 hospital admissions, totaling 157 days of hospitalization. Anakinra was initially administered during the acute phase in 2019 but was discontinued after 29 days. In 2022, the patient experienced a chronic-phase exacerbation and underwent a second course of anakinra treatment, which demonstrated a positive effect on seizure activity. With a year of anakinra therapy, the patient exhibited significant improvement in both seizure frequency and severity. This report adds to the existing evidence supporting the potential use of anakinra in the treatment of FIRES, highlighting its effectiveness during the chronic phase and suggesting the potential benefits of subsequent administration.
Full article

Figure 1
Open AccessArticle
Middle Meningeal Artery Embolization versus Surgery in Patients with Chronic Subdural Hematoma—No More Fence Sitting?
by
, , , , and
Neurol. Int. 2023, 15(4), 1480-1488; https://doi.org/10.3390/neurolint15040096 - 06 Dec 2023
Abstract
Background: Endovascular treatment of patients with chronic subdural hematoma using middle meningeal artery (MMA) embolization could become an alternative to surgical hematoma evacuation. The aim of the study was to compare methods and identify parameters to help determine the correct treatment modality. Methods:
[...] Read more.
Background: Endovascular treatment of patients with chronic subdural hematoma using middle meningeal artery (MMA) embolization could become an alternative to surgical hematoma evacuation. The aim of the study was to compare methods and identify parameters to help determine the correct treatment modality. Methods: We retrospectively reviewed 142 cases conducted internally; 78 were treated surgically and 64 were treated using MMA embolization. We analyzed the treatment failure rate and complications, and using a binary logistic regression model, we identified treatment failure risk factors. Results: We found a comparable treatment failure rate of 23.1% for the surgery group and 21.9% for the MMA embolization group. However, in the MMA embolization group, 11 cases showed treatment failure due to early neurological worsening with a need for concomitant surgery. We also found a recurrence of hematoma in 15.4% of cases in the surgery group and 6.3% of cases in the MMA embolization group. Conclusion: Both modalities have their advantages; however, correct identification is crucial for treatment success. According to our findings, hematomas with a maximal width of <18 mm, a midline shift of <5 mm, and no acute or subacute (hyperdense) hematoma could be treated with MMA embolization. Hematomas with a maximal width of >18 mm, a midline shift of >5 mm, and no membranous segmentation could have better outcomes after surgical treatment.
Full article
Open AccessArticle
Increased Susceptibility to Pilocarpine-Induced Status Epilepticus and Reduced Latency in TRPC1/4 Double Knockout Mice
Neurol. Int. 2023, 15(4), 1469-1479; https://doi.org/10.3390/neurolint15040095 - 06 Dec 2023
Abstract
►▼
Show Figures
Canonical transient receptor potential channels (TRPCs) are a family of calcium-permeable cation channels. Previous studies have shown that heteromeric channels comprising TRPC1 and TRPC4 mediate epileptiform bursting in lateral septal neurons and hippocampal CA1 pyramidal neurons, suggesting that TRPC1/4 channels play a pro-seizure
[...] Read more.
Canonical transient receptor potential channels (TRPCs) are a family of calcium-permeable cation channels. Previous studies have shown that heteromeric channels comprising TRPC1 and TRPC4 mediate epileptiform bursting in lateral septal neurons and hippocampal CA1 pyramidal neurons, suggesting that TRPC1/4 channels play a pro-seizure role. In this study, we utilized electroencephalography (EEG) recording and spectral analysis to assess the role of TRPC1/4 channels in the pilocarpine model of status epilepticus (SE). We found that, surprisingly, TRPC1/4 double knockout (DKO) mice exhibited an increased susceptibility to pilocarpine-induced SE. Furthermore, SE latency was also significantly reduced in TRPC1/4 DKO mice. Further studies are needed to reveal the underlying mechanisms of our unexpected results.
Full article

Figure 1
Open AccessArticle
Physical Rehabilitation and Post-Stroke Pneumonia: A Retrospective Observational Study Using the Japanese Diagnosis Procedure Combination Database
Neurol. Int. 2023, 15(4), 1459-1468; https://doi.org/10.3390/neurolint15040094 - 04 Dec 2023
Abstract
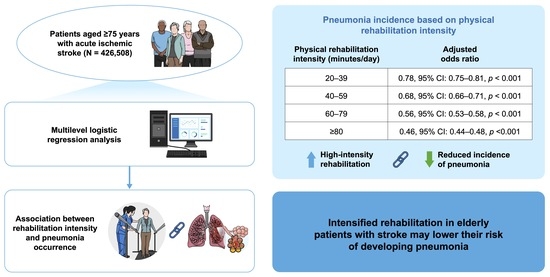
In this study, the relationship between the duration of physical rehabilitation and occurrence of pneumonia after ischemic stroke was examined. We included 426,508 patients aged
In this study, the relationship between the duration of physical rehabilitation and occurrence of pneumonia after ischemic stroke was examined. We included 426,508 patients aged
(This article belongs to the Special Issue Treatment Strategy and Mechanism of Acute Ischemic Stroke)
►▼
Show Figures
Graphical abstract
Open AccessReview
Hemorrhagic Coagulation Disorders and Ischemic Stroke: How to Reconcile Both?
Neurol. Int. 2023, 15(4), 1443-1458; https://doi.org/10.3390/neurolint15040093 - 30 Nov 2023
Abstract
Coagulation and fibrinolytic system disorders are conditions in which the blood’s ability to clot is impaired, resulting in an increased risk of thrombosis or bleeding. Although these disorders are the expression of two opposing tendencies, they can often be associated with or be
[...] Read more.
Coagulation and fibrinolytic system disorders are conditions in which the blood’s ability to clot is impaired, resulting in an increased risk of thrombosis or bleeding. Although these disorders are the expression of two opposing tendencies, they can often be associated with or be a consequence of each other, contributing to making the prognosis of acute cerebrovascular events more difficult. It is important to recognize those conditions that are characterized by dual alterations in the coagulation and fibrinolytic systems to reduce the prognostic impact of clinical conditions with difficult treatment and often unfortunate outcomes. Management of these individuals can be challenging, as clinicians must balance the need to prevent bleeding episodes with the potential risk of clot formation. Treatment decisions should be made on an individual basis, considering the specific bleeding disorder, its severity, and the patient’s general medical condition. This review aims to deal with all those forms in which coagulation and fibrinolysis represent two sides of the same media in the correct management of patients with acute neurological syndrome. Precision medicine, personalized treatment, advanced anticoagulant strategies, and innovations in bleeding control represent future directions in the management of these complex pathologies in which stroke can be the evolution of two different acute events or be the first manifestation of an occult or unknown underlying pathology.
Full article
(This article belongs to the Special Issue Treatment Strategy and Mechanism of Acute Ischemic Stroke)
►▼
Show Figures
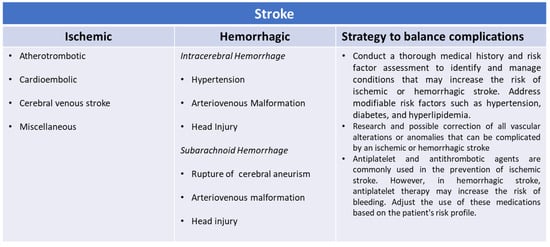
Figure 1
Open AccessReview
The Effects of Transcranial Direct Current Stimulation in Patients with Mild Cognitive Impairment
by
, , , , , , , , , , , and
Neurol. Int. 2023, 15(4), 1423-1442; https://doi.org/10.3390/neurolint15040092 - 29 Nov 2023
Abstract
►▼
Show Figures
Transcranial direct current stimulation (tDCS) came into consideration in recent years as a promising, non-invasive form of neuromodulation for individuals suffering from mild cognitive impairment (MCI). MCI represents a transitional stage between normal cognitive aging and more severe cognitive decline, which appears in
[...] Read more.
Transcranial direct current stimulation (tDCS) came into consideration in recent years as a promising, non-invasive form of neuromodulation for individuals suffering from mild cognitive impairment (MCI). MCI represents a transitional stage between normal cognitive aging and more severe cognitive decline, which appears in neurodegenerative diseases, such as Alzheimer’s disease. Numerous studies have shown that tDCS can have several useful effects in patients with MCI. It is believed to enhance cognitive functions, including memory and attention, potentially slowing down the progression of neurodegeneration and cognitive decline. tDCS is believed to work by modulating neuronal activity and promoting synaptic plasticity in the brain regions associated with cognition. Moreover, tDCS is generally considered safe and well-tolerated, making it an attractive option for long-term therapeutic use in MCI. However, further research is needed to determine the optimal stimulation parameters and long-term effects of tDCS in this population, as well as its potential to serve as a complementary therapy alongside other interventions for MCI. In this review, we included 16 randomized clinical trials containing patients with MCI who were treated with tDCS. We aim to provide important evidence for the cognitive enhancement using tDCS in patients with MCI, summarizing the effects and conclusions found in several clinical trials, and discuss its main mechanisms.
Full article

Figure 1
Open AccessArticle
Video Motion Analysis as a Quantitative Evaluation Tool for Essential Tremor during Magnetic Resonance-Guided Focused Ultrasound Thalamotomy
by
, , , , , , , , , , and
Neurol. Int. 2023, 15(4), 1411-1422; https://doi.org/10.3390/neurolint15040091 - 29 Nov 2023
Abstract
►▼
Show Figures
The Clinical Rating Scale for Tremor (CRST) is commonly used to evaluate essential tremor (ET) during focused ultrasound (FUS) thalamotomy. However, it faces challenges such as the ceiling effect and test–retest variability. This study explored the utility of videographic motion analysis as an
[...] Read more.
The Clinical Rating Scale for Tremor (CRST) is commonly used to evaluate essential tremor (ET) during focused ultrasound (FUS) thalamotomy. However, it faces challenges such as the ceiling effect and test–retest variability. This study explored the utility of videographic motion analysis as an evaluation index for ET. Forty-three patients with ET performed postural tremor and line-drawing tasks recorded on video, and the data were analyzed using motion analysis software. The test–retest and inter-rater reliability, correlations with the CRST and tremor scores, and pre/post-FUS treatment comparisons were analyzed. The video motion analysis showed excellent test–retest and inter-rater reliability. In the postural tremor tasks, video parameter amplitude significantly correlated with the CRST and tremor scores. Similarly, for the line-drawing task, video parameter amplitude showed significant correlations with CRST and tremor scores, effectively addressing the ceiling effect. Regarding post-FUS treatment improvements, changes in the CRST and tremor scores were significantly associated with changes in video parameter amplitude. In conclusion, quantitative analysis of the video motion of ET enables precise evaluation of kinematic characteristics and effectively resolves the ceiling effect and test–retest variability. The video motion analysis score accurately reflected the tremor severity and treatment effects, demonstrating its high clinical utility.
Full article

Figure 1
Open AccessCase Report
Astrocytoma Mimicking Herpetic Meningoencephalitis: The Role of Non-Invasive Multimodal Monitoring in Neurointensivism
by
, , , , , and
Neurol. Int. 2023, 15(4), 1403-1410; https://doi.org/10.3390/neurolint15040090 - 29 Nov 2023
Abstract
Neuromonitoring is a critical tool for emergency rooms and intensive care units to promptly identify and treat brain injuries. The case report of a patient with status epilepticus necessitating orotracheal intubation and intravenous lorazepam administration is presented. A pattern of epileptiform activity was
[...] Read more.
Neuromonitoring is a critical tool for emergency rooms and intensive care units to promptly identify and treat brain injuries. The case report of a patient with status epilepticus necessitating orotracheal intubation and intravenous lorazepam administration is presented. A pattern of epileptiform activity was detected in the left temporal region, and intravenous Acyclovir was administered based on the diagnostic hypothesis of herpetic meningoencephalitis. The neurointensivist opted for multimodal non-invasive bedside neuromonitoring due to the complexity of the patient’s condition. A Brain4care (B4C) non-invasive intracranial compliance monitor was utilized alongside the assessment of an optic nerve sheath diameter (ONSD) and transcranial Doppler (TCD). Based on the collected data, a diagnosis of intracranial hypertension (ICH) was made and a treatment plan was developed. After the neurosurgery team’s evaluation, a stereotaxic biopsy of the temporal lesion revealed a grade 2 diffuse astrocytoma, and an urgent total resection was performed. Research suggests that monitoring patients in a dedicated neurologic intensive care unit (Neuro ICU) can lead to improved outcomes and shorter hospital stays. In addition to being useful for patients with a primary brain injury, neuromonitoring may also be advantageous for those at risk of cerebral hemodynamic impairment. Lastly, it is essential to note that neuromonitoring technologies are non-invasive, less expensive, safe, and bedside-accessible approaches with significant diagnostic and monitoring potential for patients at risk of brain abnormalities. Multimodal neuromonitoring is a vital tool in critical care units for the identification and management of acute brain trauma as well as for patients at risk of cerebral hemodynamic impairment.
Full article
(This article belongs to the Special Issue Glioblastoma: Mechanics of Development, Progression and New Surgical and Clinical Management)
►▼
Show Figures

Figure 1
Open AccessArticle
A Characterization of Neurology Consults for Inpatients with SARS-CoV-2 Infection Compared to Other Respiratory Viruses
by
, , , , and
Neurol. Int. 2023, 15(4), 1393-1402; https://doi.org/10.3390/neurolint15040089 - 23 Nov 2023
Abstract
Introduction: Neurological consultation for patients infected with SARS-CoV-2 is common; it is currently unknown whether the neurologist’s approach to inpatient consultation of patients with SARS-CoV-2 should differ from the paradigm used to evaluate hospitalized patients with similar respiratory viruses. The goal of the
[...] Read more.
Introduction: Neurological consultation for patients infected with SARS-CoV-2 is common; it is currently unknown whether the neurologist’s approach to inpatient consultation of patients with SARS-CoV-2 should differ from the paradigm used to evaluate hospitalized patients with similar respiratory viruses. The goal of the present study is to determine if the preponderance of new neurologic diagnoses differs between inpatients with SARS-CoV-2 and similar non-SARS-CoV-2 respiratory viruses for whom neurology is consulted. Methods: We performed a retrospective chart analysis of inpatient neurologic consultations at three major Philadelphia-based hospitals. We compared the final neurologic diagnosis of 152 patients infected with SARS-CoV-2 to 54 patients with a similar ubiquitous non-SARS-CoV-2 respiratory virus (influenza A, influenza B, respiratory syncytial virus, rhinovirus, or adenovirus, the most commonly tested respiratory viruses at our institution). Secondary metrics included age, sex, level of care, prior neurologic diagnoses, and mortality. A multinomial logistic regression model was utilized to evaluate the relative difference between diagnostic category groups on all metrics. Results: The proportion of patients with seizure who were infected with SARS-CoV-2 admitted to an intensive care unit (ICU) was significantly higher than those who were admitted to a medical–surgical floor. SARS-CoV-2 was also associated with increased risk for ICU admission compared to other common respiratory viruses. SARS-CoV-2 inpatients requiring neurologic consultation were also more likely to be older and female as compared to the non-SARS-CoV-2 cohort. In other domains, the proportion of neurologic diagnoses between SAR-CoV-2 and non-SARS-CoV-2 respiratory viruses showed no significant difference. Conclusion: Patients requiring inpatient neurologic consultation with a diagnosis of SARS-CoV-2 infection or another respiratory virus were found to be remarkably similar in terms of their ultimate neurologic diagnosis, with the exception of a larger preponderance of seizure in critical-care-level patients with SARS-CoV-2 infection. Our study suggests that the neurological approach to patients hospitalized with SARS-CoV-2 should be similar to that for patients with similar common respiratory infections, noting that seizure was seen more frequently in critically ill patients infected with SARS-CoV-2.
Full article
(This article belongs to the Special Issue COVID-19, Neuroinflammation and Therapeutics)
Open AccessArticle
Characterizing the Impact of Compression Duration and Deformation-Related Loss of Closure Force on Clip-Induced Spinal Cord Injury in Rats
by
, , , , , , and
Neurol. Int. 2023, 15(4), 1383-1392; https://doi.org/10.3390/neurolint15040088 - 13 Nov 2023
Abstract
►▼
Show Figures
The clip-induced spinal cord injury (SCI) rat model is pivotal in preclinical SCI research. However, the literature exhibits variability in compression duration and limited attention to clip deformation-related loss of closure force. We aimed to investigate the impact of compression duration on SCI
[...] Read more.
The clip-induced spinal cord injury (SCI) rat model is pivotal in preclinical SCI research. However, the literature exhibits variability in compression duration and limited attention to clip deformation-related loss of closure force. We aimed to investigate the impact of compression duration on SCI severity and the influence of clip deformation on closure force. Rats received T10-level clip-induced SCI with durations of 1, 5, 10, 20, and 30 s, and a separate group underwent T10 transection. Outcomes included functional, histological, electrophysiological assessments, and inflammatory cytokine analysis. A tactile pressure mapping system quantified clip closure force after open–close cycles. Our results showed a positive correlation between compression duration and the severity of functional, histological, and electrophysiological deficits. Remarkably, even a brief 1-s compression caused significant deficits comparable to moderate-to-severe SCI. SSEP waveforms were abolished with durations over 20 s. Decreased clip closure force appeared after five open–close cycles. This study offers critical insights into regulating SCI severity in rat models, aiding researchers. Understanding compression duration and clip fatigue is essential for experiment design and interpretation using the clip-induced SCI model.
Full article

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Brain Sciences, Cancers, JCM, JVD, Neurology International
Inflammation in Neuro-Oncological Diseases and in Neuro-Vascular Diseases
Topic Editors: Erdem Güresir, Johannes Wach, Martin VychopenDeadline: 31 March 2024
Topic in
Brain Sciences, JCM, Neurology International
Neurorehabilitation in Movement Disorders and Neurodegenerative Diseases
Topic Editors: Jeff Victoroff, Neil ArchibaldDeadline: 31 December 2024
Topic in
Antioxidants, Biomolecules, JCDD, Metabolites, Neurology International, Pharmaceutics
Tissue-Specific, Disease-Signatured Macrophages in Control of Redox and Antioxidation in Metabolic Diseases
Topic Editors: Xiangwei Xiao, Yingmei Feng, Zhiyong LeiDeadline: 5 July 2025

Conferences
Special Issues
Special Issue in
Neurology International
Alpha-Synuclein in Neurological Diseases
Guest Editor: Dong Hwan HoDeadline: 31 January 2024
Special Issue in
Neurology International
Migraines and Beyond: Advances in the Pathogenesis and Treatment of Chronic Headache Disorders
Guest Editor: Yasushi ShibataDeadline: 28 February 2024
Special Issue in
Neurology International
Treatment Strategy and Mechanism of Acute Ischemic Stroke
Guest Editor: Sonu M. M. BhaskarDeadline: 1 April 2024
Special Issue in
Neurology International
COVID-19, Neuroinflammation and Therapeutics, 2nd Edition
Guest Editor: Yasir RehmanDeadline: 30 April 2024
Topical Collections
Topical Collection in
Neurology International
Brain Health Initiative: Advocacy in Global Neurology
Collection Editors: Tissa Wijeratne, Leila Karimi, Dilani Wijeratne
Topical Collection in
Neurology International
Advances in Neurodegenerative Diseases
Collection Editors: Vasileios Siokas, Efthimios Dardiotis
Topical Collection in
Neurology International
Biomarkers in Stroke Prognosis
Collection Editors: Dimitrios Tsiptsios, Konstantinos Vadikolias